Online first
Current issue
Archive
Special Issues
About the Journal
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Board
Editorial Office
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
REVIEW PAPER
The digestive system microbiome and bone: environmental determinants and health implications – a narrative review
1
Student Scientific Association at the Department of Rehabilitation, Medical University, Lublin, Poland
2
John Radcliffe Hospital, University Hospital, Oxford, United Kingdom
3
Department of Medicine of the Elderly and Stroke, Aintree University Hospital, Liverpool, United Kingdom
4
Faculty of Medicine, Gazi University, Ankara, Turkey
5
Faculty of Medicine, University of Science and Technology, Jordan
6
Faculty of Medicine, Pavel Jozef Šafárik University, Slovak Republic
7
Faculty of Science, Bilkent University, Ankara, Turkey
8
Department of Rehabilitation, Medical University, Lublin, Poland
These authors had equal contribution to this work
Corresponding author
Karolina Turzanska
Department of Rehabilitation, Medical University of Lublin, Jaczewskiego 8, 20-954, Lublin, Poland
Department of Rehabilitation, Medical University of Lublin, Jaczewskiego 8, 20-954, Lublin, Poland
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
The human microbiome is a system of microorganisms whose composition is unique to each individual. Numerous factors, including environmental and cultural factors, influence its components and their functioning. It appears that the microbiome can influence skeletal health in both positive and negative ways. The aim of the narrative review is to summarize and organize information regarding the oral and gut microbiome, probiotics, and microbiome transplantation in the context of their impact on bone health, as well as to highlight the importance of the environment in these interactions.
Review methods:
Databases such as PubMed and Google Scholar were used to search for literature. 37 articles from 2009–2023 related to the environment, the microbiome and bone health were included in the review.
Brief description of the state of knowledge:
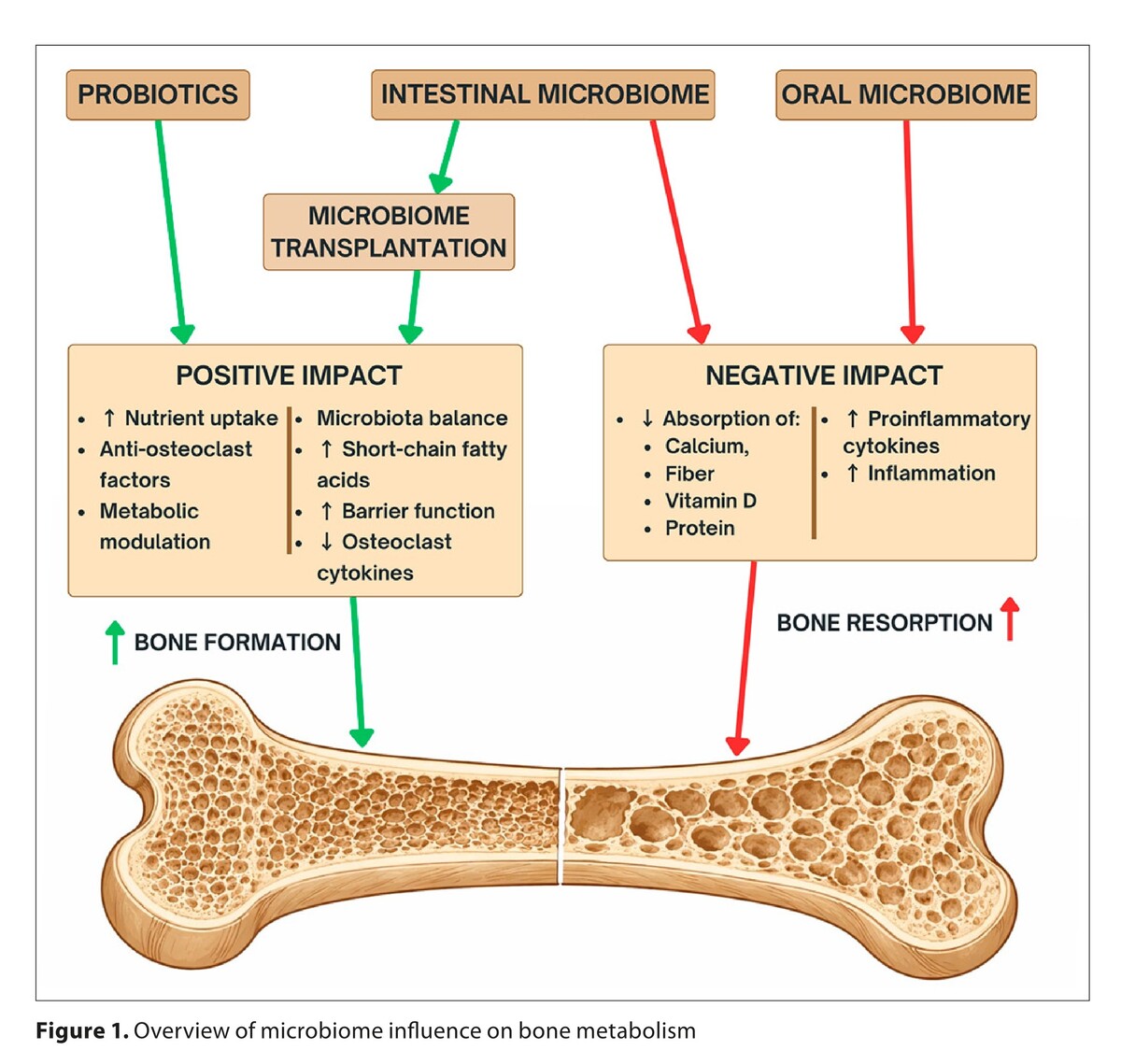
Dysbiosis and all pathologies within the oral and intestinal microbiome can contribute to poor bone health by increasing resorption processes, leading to the development of osteoporosis. Microorganisms can disrupt the proper functioning of bone tissue by impairing nutrient absorption, affecting the immune system, and modulating the gut-brain-bone axis. In turn, repairing a disrupted microbiome can be achieved through probiotic supplements and gut microbiome transplantation. Scientific studies demonstrate that these interventions are highly effective in combating these pathologies.
Summary:
Environmental and cultural factors significantly impact the development and function of microorganisms in the human body. Any dysbiosis within the microbiome can result in excessive bone resorption and the development of osteoporosis, the effects of which can be mitigated by supplementing with appropriate probiotics or by gut microbiome transplantation.
The human microbiome is a system of microorganisms whose composition is unique to each individual. Numerous factors, including environmental and cultural factors, influence its components and their functioning. It appears that the microbiome can influence skeletal health in both positive and negative ways. The aim of the narrative review is to summarize and organize information regarding the oral and gut microbiome, probiotics, and microbiome transplantation in the context of their impact on bone health, as well as to highlight the importance of the environment in these interactions.
Review methods:
Databases such as PubMed and Google Scholar were used to search for literature. 37 articles from 2009–2023 related to the environment, the microbiome and bone health were included in the review.
Brief description of the state of knowledge:
Dysbiosis and all pathologies within the oral and intestinal microbiome can contribute to poor bone health by increasing resorption processes, leading to the development of osteoporosis. Microorganisms can disrupt the proper functioning of bone tissue by impairing nutrient absorption, affecting the immune system, and modulating the gut-brain-bone axis. In turn, repairing a disrupted microbiome can be achieved through probiotic supplements and gut microbiome transplantation. Scientific studies demonstrate that these interventions are highly effective in combating these pathologies.
Summary:
Environmental and cultural factors significantly impact the development and function of microorganisms in the human body. Any dysbiosis within the microbiome can result in excessive bone resorption and the development of osteoporosis, the effects of which can be mitigated by supplementing with appropriate probiotics or by gut microbiome transplantation.
REFERENCES (49)
1.
Manos J. The human microbiome in disease and pathology. APMIS. 2022;130(12):690–705. doi:10.1111/apm.13225.
2.
de Vos WM, Tilg H, Van Hul M, Cani PD. Gut microbiome and health: mechanistic insights. Gut. 2022;71(5):1020–1032. doi:10.1136/gutjnl-2021-326789.
3.
Davenport ER, Sanders JG, Song SJ, et al. The human microbiome in evolution. BMC Biol. 2017;15(1):127. Published 2017 Dec 27. doi:10.1186/s12915-017-0454-7.
4.
Föger-Samwald U, Dovjak P, Azizi-Semrad U, et al. Osteoporosis: Pathophysiology and therapeutic options. EXCLI J. 2020;19:1017–1037. Published 2020 Jul 20. doi:10.17179/excli2020-2591.
5.
Ding K, Hua F, Ding W. Gut Microbiome and Osteoporosis. Aging Dis. 2020;11(2):438–447. Published 2020 Mar 9. doi:10.14336/AD.2019.0523.
6.
Cooney OD, Nagareddy PR, Murphy AJ, Lee MKS. Healthy Gut, Healthy Bones: Targeting the Gut Microbiome to Promote Bone Health. Front Endocrinol (Lausanne). 2021;11:620466. Published 2021 Feb 19. doi:10.3389/fendo.2020.620466.
7.
Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. Published 2021 Mar 29. doi:10.1136/bmj.n71.
8.
Lamont RJ, Koo H, Hajishengallis G. The oral microbiota: dynamic communities and host interactions. Nat Rev Microbiol. 2018;16(12):745–759. doi:10.1038/s41579-018-0089-x.
9.
Di Stefano M, Polizzi A, Santonocito S, et al. Impact of Oral Microbiome in Periodontal Health and Periodontitis: A Critical Review on Prevention and Treatment. Int J Mol Sci. 2022;23(9):5142. Published 2022 May 5. doi:10.3390/ijms23095142.
10.
Gao L, Xu T, Huang G, et al. Oral microbiomes: more and more importance in oral cavity and whole body. Protein Cell. 2018;9(5):488–500. doi:10.1007/s13238-018-0548-1.
11.
Brookes Z, Teoh L, Cieplik F, Kumar P. Mouthwash Effects on the Oral Microbiome: Are They Good, Bad, or Balanced?. Int Dent J. 2023;73 Suppl 2(Suppl 2):S74-S81. doi:10.1016/j.identj.2023.08.010.
12.
Valm AM. The Structure of Dental Plaque Microbial Communities in the Transition from Health to Dental Caries and Periodontal Disease. J Mol Biol. 2019;431(16):2957–2969. doi:10.1016/j.jmb.2019.05.016.
13.
Contaldo M, Itro A, Lajolo C, et al. Overview on Osteoporosis, Periodontitis and Oral Dysbiosis: The Emerging Role of Oral Microbiota. Applied Sci. 2020;10(17):6000. doi:10.3390/app10176000.
14.
Yu B, Wang CY. Osteoporosis and periodontal diseases – An update on their association and mechanistic links. Periodontol 2000. 2022;89(1):99–113. doi:10.1111/prd.12422.
15.
Minerbi A, Shen S. Gut Microbiome in Anesthesiology and Pain Medicine. Anesthesiol. 2022;137(1):93–108. doi:10.1097/ALN.0000000000004204.
16.
Bidell MR, Hobbs ALV, Lodise TP. Gut microbiome health and dysbiosis: A clinical primer. Pharmacotherapy. 2022;42(11):849–857. doi:10.1002/phar.2731.
17.
Adelman MW, Woodworth MH, Langelier C, et al. The gut microbiome’s role in the development, maintenance, and outcomes of sepsis. Crit Care. 2020;24(1):278. Published 2020 Jun 1. doi:10.1186/s13054-020-02989-1.
18.
Rebersek M. Gut microbiome and its role in colorectal cancer. BMC Cancer. 2021;21(1):1325. Published 2021 Dec 11. doi:10.1186/s12885-021-09054-2.
19.
Tong Y, Gao H, Qi Q, et al. High fat diet, gut microbiome and gastrointestinal cancer. Theranostics. 2021;11(12):5889–5910. Published 2021 Apr 3. doi:10.7150/thno.56157.
20.
He J, Xu S, Zhang B, et al. Gut microbiota and metabolite alterations associated with reduced bone mineral density or bone metabolic indexes in postmenopausal osteoporosis. Aging (Albany NY). 2020;12(9):8583–8604. doi:10.18632/aging.103168.
21.
Chen YC, Greenbaum J, Shen H, Deng HW. Association Between Gut Microbiota and Bone Health: Potential Mechanisms and Prospective. J Clin Endocrinol Metab. 2017;102(10):3635–3646. doi:10.1210/jc.2017-00513.
22.
Wiertsema SP, van Bergenhenegouwen J, Garssen J, Knippels LMJ. The Interplay between the Gut Microbiome and the Immune System in the Context of Infectious Diseases throughout Life and the Role of Nutrition in Optimizing Treatment Strategies. Nutrients. 2021;13(3):886. Published 2021 Mar 9. doi:10.3390/nu13030886.
23.
Locantore P, Del Gatto V, Gelli S, et al. The Interplay between Immune System and Microbiota in Osteoporosis. Mediators Inflamm. 2020;2020:3686749. Published 2020 Feb 26. doi:10.1155/2020/3686749.
24.
Wu D, Cline-Smith A, Shashkova E, et al. T-Cell Mediated Inflammation in Postmenopausal Osteoporosis. Front Immunol. 2021;12:687551. Published 2021 Jun 30. doi:10.3389/fimmu.2021.687551.
25.
Ratajczak AE, Rychter AM, Zawada A, et al. Nutrients in the Prevention of Osteoporosis in Patients with Inflammatory Bowel Diseases. Nutrients. 2020;12(6):1702. Published 2020 Jun 6. doi:10.3390/nu12061702.
26.
Bielik V, Kolisek M. Bioaccessibility and Bioavailability of Minerals in Relation to a Healthy Gut Microbiome. Int J Mol Sci. 2021;22(13):6803. Published 2021 Jun 24. doi:10.3390/ijms22136803.
27.
Zeng L, Deng Y, He Q, et al. Safety and efficacy of probiotic supplementation in 8 types of inflammatory arthritis: A systematic review and meta-analysis of 34 randomized controlled trials. Front Immunol. 2022;13:961325. Published 2022 Sep 23. doi:10.3389/fimmu.2022.961325.
28.
Rizzoli R, Biver E. Are Probiotics the New Calcium and Vitamin D for Bone Health? Curr Osteoporos Rep. 2020;18(3):273–284. doi:10.1007/s11914-020-00591-6.
29.
Arora M, Baldi A. Regulatory categories of probiotics across the globe: a review representing existing and recommended categorization. Indian J Med Microbiol. 2015;33 Suppl:2–10. doi:10.4103/0255-0857.150868.
30.
Marco ML, Tachon S. Environmental factors influencing the efficacy of probiotic bacteria. Curr Opin Biotechnol. 2013;24(2):207–213. doi:10.1016/j.copbio.2012.10.002.
31.
Hemarajata P, Versalovic J. Effects of probiotics on gut microbiota: mechanisms of intestinal immunomodulation and neuromodulation. Therap Adv Gastroenterol. 2013;6(1):39–51. doi:10.1177/1756283X12459294.
32.
Kim J, Lee E, Kim S, et al. Effects of a Lactobacillus casei 393 fermented milk product on bone metabolism in ovariectomised rats. Inter Dairy J. 2009;19: 690–695. doi:10.1016/j.idairyj.2009.06.009.
33.
Britton RA, Irwin R, Quach D, et al. Probiotic L. reuteri treatment prevents bone loss in a menopausal ovariectomized mouse model. J Cell Physiol. 2014;229(11):1822–1830. doi:10.1002/jcp.24636.
34.
Nilsson AG, Sundh D, Bäckhed F, et al. Lactobacillus reuteri reduces bone loss in older women with low bone mineral density: a randomized, placebo-controlled, double-blind, clinical trial. J Intern Med. 2018;284(3):307–317. doi:10.1111/joim.12805.
35.
Li P, Sundh D, Ji B, et al. Metabolic Alterations in Older Women With Low Bone Mineral Density Supplemented With Lactobacillus reuteri. JBMR Plus. 2021;5(4):e10478. Published 2021 Mar 15. doi:10.1002/jbm4.10478.
36.
Fijan S. Microorganisms with claimed probiotic properties: an overview of recent literature. Int J Environ Res Public Health. 2014;11(5):4745–4767. Published 2014 May 5. doi:10.3390/ijerph110504745.
37.
Porcari S, Benech N, Valles-Colomer M, et al. Key determinants of success in fecal microbiota transplantation: From microbiome to clinic. Cell Host Microbe. 2023;31(5):712–733. doi:10.1016/j.chom.2023.03.020.
38.
Zhang YW, Cao MM, Li YJ, et al. Fecal microbiota transplantation as a promising treatment option for osteoporosis. J Bone Miner Metab. 2022;40(6):874–889. doi:10.1007/s00774-022-01375-x.
39.
Greyson-Gaito CJ, Bartley TJ, Cottenie K, et al. Into the wild: microbiome transplant studies need broader ecological reality. Proc Biol Sci. 2020;287(1921):20192834. doi:10.1098/rspb.2019.2834.
40.
Kelly CR, Yen EF, Grinspan AM, et al. Fecal Microbiota Transplantation Is Highly Effective in Real-World Practice: Initial Results From the FMT National Registry. Gastroenterol. 2021;160(1):183–192.e3. doi:10.1053/j.gastro.2020.09.038.
41.
Ma S, Wang N, Zhang P, et al. Fecal microbiota transplantation mitigates bone loss by improving gut microbiome composition and gut barrier function in aged rats. Peer J. 2021;9:e12293. Published 2021 Oct 21. doi:10.7717/peerj.12293.
42.
Wang N, Ma S, Fu L. Gut Microbiota Dysbiosis as One Cause of Osteoporosis by Impairing Intestinal Barrier Function. Calcif Tissue Int. 2022;110(2):225–235. doi:10.1007/s00223-021-00911-7.
43.
Zhang YW, Cao MM, Li YJ, et al. Fecal microbiota transplantation ameliorates bone loss in mice with ovariectomy-induced osteoporosis via modulating gut microbiota and metabolic function. J Orthop Translat. 2022;37:46–60. Published 2022 Sep 26. doi:10.1016/j.jot.2022.08.003.
44.
Ramai D, Zakhia K, Ofosu A, et al. Fecal microbiota transplantation: donor relation, fresh or frozen, delivery methods, cost-effectiveness. Ann Gastroenterol. 2019;32(1):30–38. doi:10.20524/aog.2018.0328.
45.
Ng SC, Kamm MA, Yeoh YK, et al. Scientific frontiers in faecal microbiota transplantation: joint document of Asia-Pacific Association of Gastroenterology (APAGE) and Asia-Pacific Society for Digestive Endoscopy (APSDE). Gut. 2020;69(1):83–91. doi:10.1136/gutjnl-2019-319407.
46.
Wang Y, Zhang S, Borody TJ, Zhang F. Encyclopedia of fecal microbiota transplantation: a review of effectiveness in the treatment of 85 diseases. Chin Med J (Engl). 2022;135(16):1927–1939. Published 2022 Aug 20. doi:10.1097/CM9.0000000000002339.
47.
Wang W, Lu G, Wu X, et al. Colonic Transendoscopic Enteral Tubing Is a New Pathway to Microbial Therapy, Colonic Drainage, and Host-Microbiota Interaction Research. J Clin Med. 2023;12(3):780. Published 2023 Jan 18. doi:10.3390/jcm12030780.
48.
Huang YF, Chang CT, Liu SP, et al. The Impact of Oral Hygiene Maintenance on the Association Between Periodontitis and Osteoporosis: A Nationwide Population-Based Cross Sectional Study. Medicine (Baltimore). 2016;95(6):e2348. doi:10.1097/MD.0000000000002348.
49.
Gregori G, Pivodic A, Magnusson P, et al. Limosilactobacillus reuteri 6475 and Prevention of Early Postmenopausal Bone Loss: A Randomized Clinical Trial. JAMA Netw Open. 2024;7(6):e2415455. Published 2024 Jun 3. doi:10.1001/jamanetworkopen.2024.15455.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.