Online first
Current issue
Archive
Special Issues
About the Journal
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Board
Editorial Office
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
RESEARCH PAPER
The diagnostic value of miR-1-3p in atopic dermatitis and its correlation with inflammatory factors
1
Department of Cosmetic Dermatology, Zigong Fourth People’s Hospital, China
2
Department of Dermatology and Venereology, Sir Run Run Shaw Hospital, Zhejiang University School of Medicine, China
3
Department of Plastic Surgery, The Second Hospital of Hebei Medical University, China
4
Department of Laboratory Medicine, The Second People’s Hospital of Chun’an County (Chun’an Branch of Affiliated Hospital of Hangzhou Normal University), China
Corresponding author
Juan Wang
Department of Laboratory Medicine, The Second People’s Hospital of Chun’an County (Chun’an Branch of Affiliated Hospital of Hangzhou Normal University), Hangzhou 311719, China, China
Department of Laboratory Medicine, The Second People’s Hospital of Chun’an County (Chun’an Branch of Affiliated Hospital of Hangzhou Normal University), Hangzhou 311719, China, China
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
MicroRNAs (miRNAs), such as miR-1-3p, play a crucial role in inflammatory processes, including atopic dermatitis (AD). The aim of the study is to investigate the role of miR-1-3p in AD, and its correlation with inflammation.
Material and methods:
miR-1-3p level was analyzed using qRT-PCR. Its diagnostic value was assessed via ROC curve analysis. Correlations between miR-1-3p and inflammatory factors were assessed by Spearman’s rank correlation coefficient. Proliferation of HaCaT cells were detected by CCK-8. The influence of miR-1-3p for inflammatory factors were examined through enzyme-linked immunosorbent assay (ELISA). Target genes of miR-1-3p were predicted using bioinformatics databases.
Results:
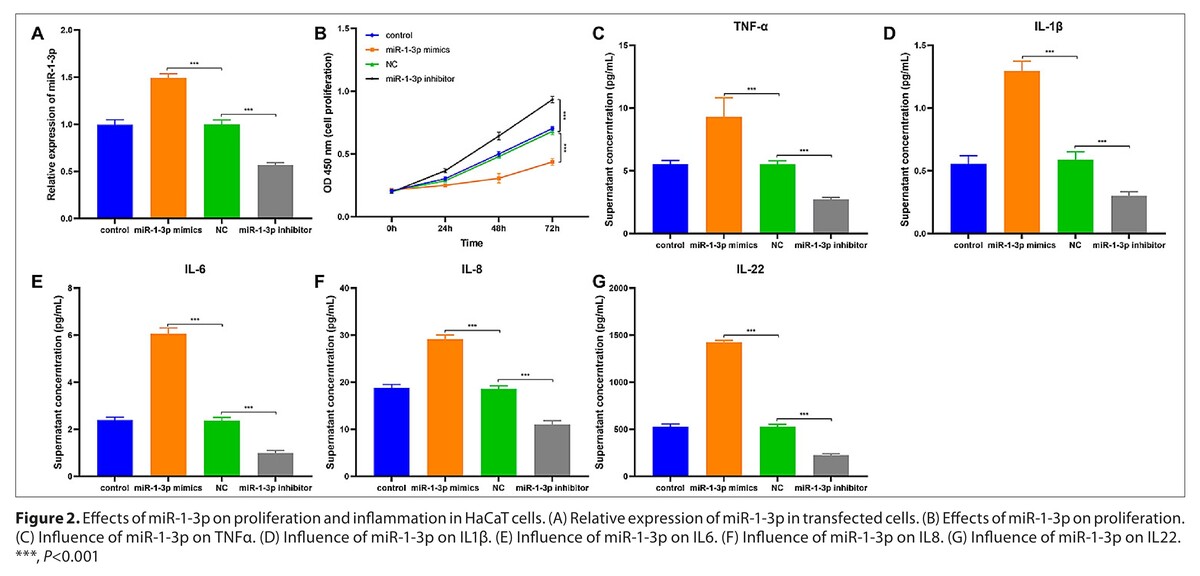
miR-1-3p was upregulated in AD patients and had a high diagnostic value (area under ROC curve=0.927, sensitivity=0.830, specificity=0.934) for AD. miR-1-3p was negatively correlated with lymphocytes (r=-0.558), and positively correlated with CRP (r=0.570), IL-6 (r=0.511), and IL-22 (r=0.596) levels, respectively. A high miR-1-3p level in HaCaT cells suppressed proliferation and increased inflammatory cytokine levels. Bioinformatics analysis identified 61 ovrerlapping target genes of miR-1-3p, enriched in pathways associated with inflammation and immune response.
Conclusions:
miR-1-3p is elevated in AD and associated with inflammation, suggesting a role in AD pathogenesis. Its effects on HaCaT cells and correlation with inflammatory markers indicate a mechanistic involvement in AD.
MicroRNAs (miRNAs), such as miR-1-3p, play a crucial role in inflammatory processes, including atopic dermatitis (AD). The aim of the study is to investigate the role of miR-1-3p in AD, and its correlation with inflammation.
Material and methods:
miR-1-3p level was analyzed using qRT-PCR. Its diagnostic value was assessed via ROC curve analysis. Correlations between miR-1-3p and inflammatory factors were assessed by Spearman’s rank correlation coefficient. Proliferation of HaCaT cells were detected by CCK-8. The influence of miR-1-3p for inflammatory factors were examined through enzyme-linked immunosorbent assay (ELISA). Target genes of miR-1-3p were predicted using bioinformatics databases.
Results:
miR-1-3p was upregulated in AD patients and had a high diagnostic value (area under ROC curve=0.927, sensitivity=0.830, specificity=0.934) for AD. miR-1-3p was negatively correlated with lymphocytes (r=-0.558), and positively correlated with CRP (r=0.570), IL-6 (r=0.511), and IL-22 (r=0.596) levels, respectively. A high miR-1-3p level in HaCaT cells suppressed proliferation and increased inflammatory cytokine levels. Bioinformatics analysis identified 61 ovrerlapping target genes of miR-1-3p, enriched in pathways associated with inflammation and immune response.
Conclusions:
miR-1-3p is elevated in AD and associated with inflammation, suggesting a role in AD pathogenesis. Its effects on HaCaT cells and correlation with inflammatory markers indicate a mechanistic involvement in AD.
REFERENCES (25)
1.
Asthma GBD, Allergic Diseases C. Global, regional, and national burden of asthma and atopic dermatitis, 1990–2021, and projections to 2050: a systematic analysis of the Global Burden of Disease Study 2021. Lancet Respir Med. 2025;13(5):425–46. https://doi.org/10.1016/S2213-....
2.
Qian X, Tong M, Zhang T, et al. IL-24 promotes atopic dermatitis-like inflammation through driving MRSA-induced allergic responses. Protein Cell. 2025;16(3):188–210. https://doi.org/10.1093/procel....
3.
Kim HB, Alexander H, Um JY, et al. Skin Microbiome Dynamics in Atopic Dermatitis: Understanding Host-Microbiome Interactions. Allergy Asthma Immunol Res. 2025;17(2):165–80. https://doi.org/10.4168/aair.2....
4.
Boothe WD, Tarbox JA, Tarbox MB. Atopic Dermatitis: Pathophysiology. Adv Exp Med Biol. 2024;1447:21–35. https://doi.org/10.1007/978-3-....
5.
Dezoteux F, Marcant P, Dendooven A, et al. Enhanced Siglec-8 and HLA-DR and reduced CRTH2 surface expression highlight a distinct phenotypic signature of circulating eosinophils in atopic dermatitis. J Leukoc Biol. 2025;117(4). https://doi.org/10.1093/jleuko....
6.
Huang D, Liu X, Gao X, et al. Meteorin-like protein/METRNL/Interleukin-41 ameliorates atopic dermatitis-like inflammation. Allergy. 2025;80(2):474–88. https://doi.org/10.1111/all.16....
7.
Zhang X, Li J, Liu Y, et al. Myricetin alleviates DNCB-induced atopic dermatitis by modulating macrophage M1/M2 polarization. Int Immunopharmacol. 2025;163:115212. https://doi.org/10.1016/j.inti....
8.
Gage D, Ma EZ, Fayyad D, et al. Clustering analysis of circulating plasma-biomarkers in atopic dermatitis reveals a distinct-inflammatory cardiac risk profile in African American patients. Res Sq. 2025. https://doi.org/10.21203/rs.3.....
9.
Vasku V, Vasku A. Several Proinflammatory Genes’ Variability and Phenotypes of Atopic Dermatitis in Czech Adult AD Patients. Genes (Basel). 2025;16(6). https://doi.org/10.3390/genes1....
10.
D’Avino P, Kim J, Li M, et al. Distinct Roles of IL-4, IL-13, and IL-22 in Human Skin Barrier Dysfunction and Atopic Dermatitis. Allergy. 2025. https://doi.org/10.1111/all.70....
11.
Kang KM, Han JH, Kim KS, et al. Chlorophyll a and novel synthetic derivatives alleviate atopic dermatitis by suppressing Th2 cell differentiation via IL-4 receptor modulation. Clin Immunol. 2024;258:109852. https://doi.org/10.1016/j.clim....
12.
Schiavello M, Bosco O, Vizio B, et al. Profiling of miRNAs Contained in Circulating Extracellular Vesicles and Associated with Sepsis Development in Burn Patients: A Proof-of-Concept Study. Int J Mol Sci. 2025;26(5). https://doi.org/10.3390/ijms26....
13.
Deng C, Huo M, Chu H, et al. Exosome circATP8A1 induces macrophage M2 polarization by regulating the miR-1-3p/STAT6 axis to promote gastric cancer progression. Mol Cancer. 2024;23(1):49. https://doi.org/10.1186/s12943....
14.
Mao J, Gai Q, Bao X, Zhong M. From miRNA sponges to mTOR blockades: mapping the multidimensional landscape of ameloblastoma pathogenesis and precision targeting. Front Oncol. 2025;15:1651236. https://doi.org/10.3389/fonc.2....
15.
Luo H, Wu Z-h, Zhong J, Zhang Y, Feng G. MicroRNAs with differential expression between atopic dermatitis and psoriasis and their biological function Guangxi Medical Journal. 2020;42(17):2257–63. https://doi.org/10.11675/j.iss....
16.
Williams HC, Burney PG, Hay RJ, et al. The U.K. Working Party’s Diagnostic Criteria for Atopic Dermatitis. I. Derivation of a minimum set of discriminators for atopic dermatitis. Br J Dermatol. 1994;131(3):383–96. https://doi.org/10.1111/j.1365....
17.
Chopra R, Vakharia PP, Sacotte R, et al. Severity strata for Eczema Area and Severity Index (EASI), modified EASI, Scoring Atopic Dermatitis (SCORAD), objective SCORAD, Atopic Dermatitis Severity Index and body surface area in adolescents and adults with atopic dermatitis. Br J Dermatol. 2017;177(5):1316–21. https://doi.org/10.1111/bjd.15....
18.
Khosrojerdi M, Azad FJ, Yadegari Y, et al. The role of microRNAs in atopic dermatitis. Noncoding RNA Res. 2024;9(4):1033–9. https://doi.org/10.1016/j.ncrn....
19.
Li L, Ma X, Zhao YF, Zhang C. MiR-1-3p facilitates Th17 differentiation associating with multiple sclerosis via targeting ETS1. Eur Rev Med Pharmacol Sci. 2020;24(12):6881–92. https://doi.org/10.26355/eurre....
20.
Nemati Bajestan M, Piroozkhah M, Chaleshi V, et al. Expression Analysis of Long Noncoding RNA-MALAT1 and Interleukin-6 in Inflammatory Bowel Disease Patients. Iran J Allergy Asthma Immunol. 2023;22(5):482–94. https://doi.org/10.18502/ijaai....
21.
Bakker D, de Bruin-Weller M, Drylewicz J, et al. Biomarkers in atopic dermatitis. J Allergy Clin Immunol. 2023;151(5):1163–8. https://doi.org/10.1016/j.jaci....
22.
Xu M, Sun J, Yu Y, et al. TM4SF1 involves in miR-1-3p/miR-214-5p-mediated inhibition of the migration and proliferation in keloid by regulating AKT/ERK signaling. Life Sci. 2020;254:117746. https://doi.org/10.1016/j.lfs.....
23.
Hua W, Li M, Yan Z, et al. Kaempferol prevents Nrf2 from ubiquitin-mediated proteolysis to mitigate both NLRP3 inflammation and oxidative stress: implications for alleviating DSS-induced colitis in mice. Inflammopharmacol. 2025;33(11):6861–76. https://doi.org/10.1007/s10787....
24.
Li R, Ma Y, Wu H, et al. 4-Octyl itaconate alleviates endothelial cell inflammation and barrier dysfunction in LPS-induced sepsis via modulating TLR4/MAPK/NF-kappaB signaling: 4-Octyl itaconate alleviates endothelial dysfunction. Mol Med. 2025;31(1):240. https://doi.org/10.1186/s10020....
25.
Zhang Z, Zhou M, Tang Y, et al. Impaired megakaryopoiesis due to aberrant macrophage polarization via BTK/Rap1/NF-kappaB pathway in sepsis-induced thrombocytopenia. Mol Ther. 2025;33(4):1769–84. https://doi.org/10.1016/j.ymth....
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.