Online first
Current issue
Archive
Special Issues
About the Journal
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Board
Editorial Office
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
RESEARCH PAPER
Quality of life among patients from urban and rural areas with advanced age-related macular degeneration assessed using the NEI-VFQ-25
1
Department of Vitreoretinal Surgery, Medical University, Lublin, Poland
2
Department Diagnostics and Microsurgery of Glaucoma, Medical University, Lublin, Poland
Corresponding author
Anna Święch
Klinika Chirurgii Siatkówki i Ciała Szklistego Katedry Okulistyki 20-079 Lublin ul. Chmielna 1 (SPSK NR 1) +48 81534 0251, Poland
Klinika Chirurgii Siatkówki i Ciała Szklistego Katedry Okulistyki 20-079 Lublin ul. Chmielna 1 (SPSK NR 1) +48 81534 0251, Poland
Ann Agric Environ Med. 2021;28(2):243-249
KEYWORDS
TOPICS
- Biological agents posing occupational risk in agriculture, forestry, food industry and wood industry and diseases caused by these agents (zoonoses, allergic and immunotoxic diseases)
- State of the health of rural communities depending on various factors: social factors, accessibility of medical care, etc.
ABSTRACT
Objective:
The aim of the study was to explore the influence of exudative age-related macular degeneration on the quality of life of patients from urban and rural areas.
Material and methods:
The retrospective study included 144 Polish Caucasians with exudative age-related macular degeneration, treated with anti-VEGF, recruited from Department of Medical Retina in Lublinbetween March and June 2017. Clinical assessment included age, gender, visual acuity, complete ophthalmic examination, fundus fluorescein angiography and optical coherence tomography, medical history and the NEI VFQ-25 questionnaire.
Results:
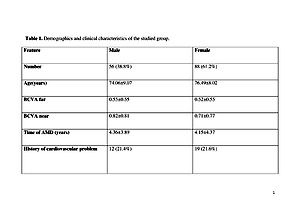
The mean age of the study group was 76.73±12.3 years, average time of AMD was 4.24±4.1 years. 21.5% of patients reported comorbidities such as hypertension, cardiovascular disease, diabetes mellitus. 99 (68.75%) lived in a city, while 45(31.25%) in a village. There was a tendency of females to complain more than males about moderate and severe discomfort and pain (p = 0.09). Most of the patients did not drive a car before the onset of the disease (female vs.male: 81% vs 62.9%; p = 0.01). 62.8% males and 25.8% females gave up driving (p = 0.003), whereas significantly more males gave up driving’ and 25% of villagers gave up driving (p = 0.07). The parameter because of the eyesight – female vs. male: 50% vs. 20.8%; p = 0.03. There was a tendency of village respondents to complain more often about extreme difficulty in reading newspapers, street signs or the names of stores than (p = 0.08). 44.2% city residents. Rural patients felt to achieve much less because of their eyesight, which was not observed in patients from the city (p = 0.06).
Conclusions:
The place of residence and gender influenced perception of the disease in exudative form of age-related macular degeneration.
The aim of the study was to explore the influence of exudative age-related macular degeneration on the quality of life of patients from urban and rural areas.
Material and methods:
The retrospective study included 144 Polish Caucasians with exudative age-related macular degeneration, treated with anti-VEGF, recruited from Department of Medical Retina in Lublinbetween March and June 2017. Clinical assessment included age, gender, visual acuity, complete ophthalmic examination, fundus fluorescein angiography and optical coherence tomography, medical history and the NEI VFQ-25 questionnaire.
Results:
The mean age of the study group was 76.73±12.3 years, average time of AMD was 4.24±4.1 years. 21.5% of patients reported comorbidities such as hypertension, cardiovascular disease, diabetes mellitus. 99 (68.75%) lived in a city, while 45(31.25%) in a village. There was a tendency of females to complain more than males about moderate and severe discomfort and pain (p = 0.09). Most of the patients did not drive a car before the onset of the disease (female vs.male: 81% vs 62.9%; p = 0.01). 62.8% males and 25.8% females gave up driving (p = 0.003), whereas significantly more males gave up driving’ and 25% of villagers gave up driving (p = 0.07). The parameter because of the eyesight – female vs. male: 50% vs. 20.8%; p = 0.03. There was a tendency of village respondents to complain more often about extreme difficulty in reading newspapers, street signs or the names of stores than (p = 0.08). 44.2% city residents. Rural patients felt to achieve much less because of their eyesight, which was not observed in patients from the city (p = 0.06).
Conclusions:
The place of residence and gender influenced perception of the disease in exudative form of age-related macular degeneration.
Święch A, Dolar-Szczasny J, Wróbel-Dudzińska D, Kosior-Jarecka E, Mackiewicz J. Quality of life among patients from urban and rural areas with advanced age-related macular degeneration assessed using the NEI-VFQ-25. Ann Agric Environ Med. Doi: 10.26444/aaem/130436
REFERENCES (13)
1.
Ćwirlej-Sozańska A, Sozański B, Wiśniowska-Szurlej A, Wilmowska-Pietruszyńska A. Quality of life and related factors among older people living in rural areas in south-eastern Poland. Ann Agric Environ Med. 2018; 25(3): 539–545. doi: 10.26444/aaem/93847.
2.
Orr P, Rentz AM, Margolis MK, Revicki DA, Dolan CM, Bressler NM, et al. Validation of the National Eye Institute Visual Function Questionnaire-25 (NEI VFQ-25) in age-related macular degeneration. Invest Ophthalmol Vis Sci. 2011; 52(6): 3354–3359. doi: 10.1167/iovs.10-5645.
3.
Xu K, Gupta V, Bae S, Sharma S. Metamorphopsia and vision-related quality of life among patients with age-related macular degeneration. Can J Ophthalmol. 2018; 53(2): 168–172. doi: 10.1016/j.jcjo.2017.08.006.
4.
Riva I, Legramandi L, Rulli E, Konstas AG, Katsanos A, Quaranta L, Italian Study Group On Qol, et al. Vision-related quality of life and symptom perception change over time in newly-diagnosed primary open angle glaucoma patients. Glaucoma. Sci Rep. 2019; 9(1): 6735. doi: 10.1038/s41598-019-43203-9.
5.
Age-Related Eye Disease Study Research Group. The Age-Related Eye Disease Study (AREDS): design implications. AREDS report no. 1. Control Clin Trials. 1999; 20(6): 573–600. doi: 10.1016/s0197-2456(99)00031-8.
6.
Nordmann JP, Viala M, Sullivan K, Arnould B, Berdeaux G. Psychometric Validation of the National Eye Institute Visual Function Questionnaire – 25 (NEI VFQ-25) French version: in a population of patients treated for ocular hypertension and glaucoma. Pharmacoeconomics. 2004; 22(3): 197–206. doi: 10.2165/00019053-200422030-00005.
7.
Yang L, Shi X, Tang X. Associations of subjective and objective clinical outcomes of visual functions with quality of life in Chinese glaucoma patients: a cross-sectional study. BMC Ophthalmol. 2019; 19(1): 166. doi: 10.1186/s12886-019-1176-0.
8.
Inan S, Cetinkaya E, Duman R, Dogan I, Inan UÜ. Quality of life among patients with age-related severe macular degeneration assessed using the NEI-VFQ, HADS-A, HADS-D and SF-36 tests. A cross-sectional study. Sao Paulo Med. 2019; 137(1): 15–32. doi: 10.1590/1516-3180.2018.0195071218.
9.
Lane J, Rohan EMF, Sabeti F, Essex RW, Maddess T, McKone E, et al. Impacts of impaired face perception on social interactions and quality of life in age-related macular degeneration: A qualitative study and new community resources. PLoS One. 2018; 13(12): e0209218. doi: 10.1371/journal.pone.0209218.
10.
Mangione CM, Lee PP, Gutierrez PR, Spritzer K, Berry S, National Eye Institute Visual Function Questionnaire Field Test Investigators, et al. Development of the 25-item National Eye Institute Visual Function. Arch Ophthalmol. 2001; 119: 1050–1058. doi: 10.1001/archopht.119.7.1050.
11.
Roh M, Selivanova A, Shin HJ, Miller JW, Jackson ML. Visual acuity and contrast sensitivity are two important factors affecting vision-related quality of life in advanced age-related macular degeneration. PLoS One. 2018; 13(5): 471–75. doi: 10.1371/journal.pone.0196481.
12.
Ryu SJ, Lee WJ, Tarver LB, Shin YU, Kang MH, Cho HY, et al. Depressive Symptoms and Quality of Life in Age-related Macular Degeneration Based on Korea National Health and Nutrition Examination Survey (KNHANES). Korean J Ophthalmol. 2017; 3(5): 413–423. https://doi.org/10.3341/kjo.20....
13.
Bian W, Wan J, Smith G, Li S, Tan M, Zhou F. Domains of health-related quality of life in age-related macular degeneration: a qualitative study in the Chinese cultural context. BMJ Open. 2018; 8(4): e018756. doi: 10.1136/bmjopen-2017-018756.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.