Online first
Current issue
Archive
Special Issues
About the Journal
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Board
Editorial Office
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
RESEARCH PAPER
Lifestyle intervention towards Mediterranean Diet, physical activity adherence and anthropometric parameters in normal weight women with Polycystic Ovary Syndrome or Hashimoto’s Thyroiditis – preliminary study
1
Student Scientific Group of Hygiene and Prevention, Department of Social Medicine and Public Health, Medical University, Warsaw, Poland
2
Department of Social Medicine and Public Health, Medical University, Warsaw, Poland
Corresponding author
Katarzyna Okręglicka
Department of Social Medicine and Public Health, Medical University of Warsaw, ul. Oczki 3/213, 02-007, Warszawa, Poland
Department of Social Medicine and Public Health, Medical University of Warsaw, ul. Oczki 3/213, 02-007, Warszawa, Poland
Ann Agric Environ Med. 2023;30(1):111-117
KEYWORDS
TOPICS
ABSTRACT
Introduction:
Overweight and obesity are frequently present in both women with polycystic ovary syndrome (PCOS) and with Hashimoto’s thyroiditis (HT). This is a limited study regarding the benefits of lifestyle changes, including dietary habits, dedicated to patients with HT and PCOS.
Objective:
The aim of the study was to assess the effectiveness of an intervention programme based on the Mediterranean Diet (MD) without caloric restriction and increased physical activity to change selected anthropometric parameters in women with both health conditions.
Material and methods:
The intervention programme consisted of changing the participants diet towards MD rules and increasing physical activity for 10 weeks according WHO recommendation. The study involved 14 women diagnosed with HT, 15 with PCOS and 24 women from a control group. The intervention programme consisted of educating patients in the form of a lecture, dietary advice, leaflets and a 7-day menu based on MD. During the programme, patients were required to implement recommended lifestyle changes. The mean intervention time was 72 ± 20 days. Nutritional status was analyzed by body composition, degree of implementation of the principles of the MD by using the MedDiet Score Tool, and the level of physical activity by the IPAQ-PL questionnaire. The above-mentioned parameters were evaluated twice, before and after the intervention.
Results:
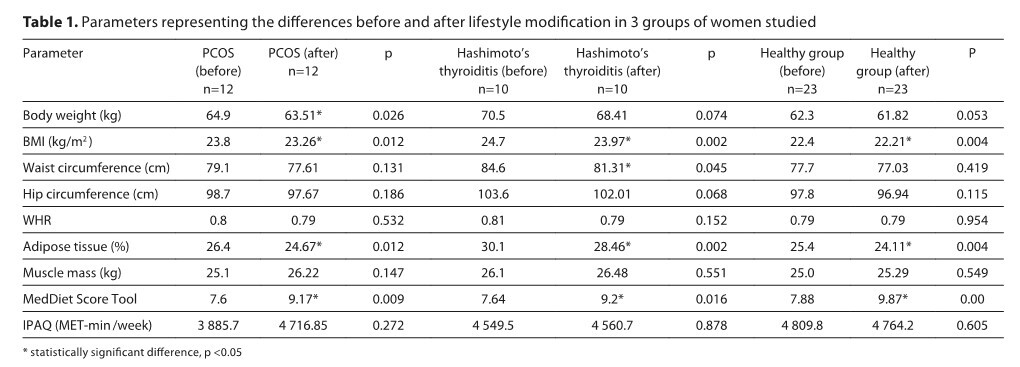
The intervention programme consisting in implementing the principles of the MD and increasing physical activity to effect a change in the anthropometric parameters of all groups of women studied; all women had a reduction in body fat and body mass index. A decrease in waist circumference was observed in the group of patients with Hashimoto’s disease.
Conclusions:
An intervention programme based on the Mediterranean Diet and physical activity can be a good way to improve the health of HT and PCOS patients.
Overweight and obesity are frequently present in both women with polycystic ovary syndrome (PCOS) and with Hashimoto’s thyroiditis (HT). This is a limited study regarding the benefits of lifestyle changes, including dietary habits, dedicated to patients with HT and PCOS.
Objective:
The aim of the study was to assess the effectiveness of an intervention programme based on the Mediterranean Diet (MD) without caloric restriction and increased physical activity to change selected anthropometric parameters in women with both health conditions.
Material and methods:
The intervention programme consisted of changing the participants diet towards MD rules and increasing physical activity for 10 weeks according WHO recommendation. The study involved 14 women diagnosed with HT, 15 with PCOS and 24 women from a control group. The intervention programme consisted of educating patients in the form of a lecture, dietary advice, leaflets and a 7-day menu based on MD. During the programme, patients were required to implement recommended lifestyle changes. The mean intervention time was 72 ± 20 days. Nutritional status was analyzed by body composition, degree of implementation of the principles of the MD by using the MedDiet Score Tool, and the level of physical activity by the IPAQ-PL questionnaire. The above-mentioned parameters were evaluated twice, before and after the intervention.
Results:
The intervention programme consisting in implementing the principles of the MD and increasing physical activity to effect a change in the anthropometric parameters of all groups of women studied; all women had a reduction in body fat and body mass index. A decrease in waist circumference was observed in the group of patients with Hashimoto’s disease.
Conclusions:
An intervention programme based on the Mediterranean Diet and physical activity can be a good way to improve the health of HT and PCOS patients.
REFERENCES (31)
1.
Uhliarova B, Hajtman A. Hashimoto’s thyroiditis – an independent risk factor for papillary carcinoma. Braz J Otorhinolaryngol. 2018;84(6):729–35. https://doi.org/10.1016/j.bjor....
2.
Ragusa F, Fallahi P, Elia G, et al. Hashimotos’ thyroiditis: Epidemiology, pathogenesis, clinic and therapy. Best Pract Res Clin Endocrinol Metab. 2019;33(6):101367. https://doi.org/10.1016/j.beem....
3.
Ralli M, Angeletti D, Fiore M, et al. Hashimoto’s thyroiditis: An update on pathogenic mechanisms, diagnostic protocols, therapeutic strategies, and potential malignant transformation. Autoimmun Rev. 2020;19(10):102649. https://doi.org/10.1016/j.autr....
4.
Liontiris MI, Mazokopakis EE. A concise review of Hashimoto thyroiditis (HT) and the importance of iodine, selenium, vitamin D and gluten on the autoimmunity and dietary management of HT patients.Points that need more investigation. Hell J Nucl Med. 2017;20(1):51–56. https://doi.org/10.1967/s00244....
5.
Weetman AP. An update on the pathogenesis of Hashimoto’s thyroiditis. J Endocrinol Invest. 2021;44(5):883–890. https://doi.org/10.1007/s40618....
6.
Sanyal D, Raychaudhuri M. Hypothyroidism and obesity: An intriguing link. Indian J Endocrinol Metab. 2016;20(4):554–7. https://doi.org/10.4103/2230-8....
7.
Walczak K, Sieminska L. Obesity and Thyroid Axis. Int J Environ Res Public Health. 2021;7(18):9434. https://doi.org/10.3390/ijerph....
8.
Radetti G, Longhi S, Baiocchi M, et al. Changes in lifestyle improve body composition, thyroid function, and structure in obese children. J Endocrinol Invest. 2012;35(3):281–5. https://doi.org/10.3275/7763.
9.
Delitala AP, Capobianco G, Delitala G, et al. Polycystic ovary syndrome, adipose tissue and metabolic syndrome. Arch Gynecol Obstet. 2017;296(3):405–19. https://doi.org/10.1007/s00404....
10.
Astapova O, Minor BMN, Hammes SR. Physiological and Pathological ndrogen Actions in the Ovary. Endocrinology. 2019;160(5):1166–1174. https://doi.org/10.1210/en.201....
11.
Escobar-Morreale HF. Polycystic ovary syndrome: definition, aetiology, diagnosis and treatment. Nat Rev Endocrinol. 2018;14(5):270–84. https://doi.org/10.1038/nrendo....
12.
Domecq JP, Prutsky G, Mullan RJ, et al. Lifestyle Modification Programmes in Polycystic Ovary Syndrome: Systematic Review and Meta-Analysis. J Clin Endocrinol Metab. 2013;98(12):4655–63. https://doi.org/10.1210/jc.201....
13.
Nath C, Barman B, Das A, et al. Prolactin and thyroid stimulating hormone affecting the pattern of LH/FSH secretion in patients with polycystic ovary syndrome: A hospital-based study from North East India. J Fam Med Prim Care. 2019;8(1):256. https://doi.org/10.4103/jfmpc.....
14.
Almenning I, Rieber-Mohn A, Lundgren KM, et al. Effects of High Intensity Interval Training and Strength Training on Metabolic, Cardiovascular and Hormonal Outcomes in Women with Polycystic Ovary Syndrome: A Pilot Study. PLoS One. 2015;10(9):e0138793. https://doi.org/10.1371/journa....
15.
Silvestrim RL, Bos-Mikich A, Kulmann MIR, et al. The Effects of Overweight and Obesity on Assisted Reproduction Technology Outcomes. JBRA Assist Reprod. 2019;23(3):281. https://doi.org/10.5935/1518-0....
16.
Tosti V, Bertozzi B, Fontana L. Health Benefits of the Mediterranean Diet: Metabolic and Molecular Mechanisms. J Gerontol Ser A. 2018;73(3):318–26. https://doi.org/10.1093/gerona....
17.
Martínez-González MÁ, Hershey MS, Zazpe I, et al. Transferability of the Mediterranean Diet to Non-Mediterranean Countries. What Is and What Is Not the Mediterranean Diet. Nutrients. 2017;9(11):1226. https://doi.org/10.3390/nu1007....
18.
Muscogiuri G, Palomba S, Lagana A, et al. Current Insights Into Inositol Isoforms, Mediterranean and Ketogenic Diets for Polycystic Ovary Syndrome: From Bench to Bedside. Curr Pharm Des. 2016;22(36):5554-7. https://doi.org/10.2174/138161....
19.
World Health Organization. Waist Circumference and Waist–Hip Ratio: Report of a WHO Expert Consultation, Geneva, 8–11 December 2008.Geneva, Switzerland: World Health Organization; 2011.
20.
Martínez-González M, García-Arellano A, Toledom E, et al. A 14-item Mediterranean diet assessment tool and obesity indexes among high-risk subjects: the PREDIMED trial. PLoS One. 2012;7(8):e43134. doi: 10.1371/journal.pone.0043134.
21.
Biernat E, Stupnicki R, Gajewski AK. Międzynarodowy Kwestionariusz Aktywności Fizycznej (IPAQ)–wersja polska. Wychowanie Fizyczne i Sport. 2007;51(1):47–54.
22.
Biernat E, Stupnicki R, Piłsudski J, et al. International Physical Activity Questionnaire (IPAQ)-Polish version View project The role of sports activity in building social capital in Poland View project. Public Health. 2016;13(8):798.
23.
Physical status: the use and interpretation of anthropometry. Report of a WHO Expert Committee. World Health Organ Tech Rep Ser. 1995;854:1–452.
24.
Jackson SE, Llewellyn CH, Smith L. The obesity epidemic–Nature via nurture: A narrative review of high-income countries. SAGE Open Med. 2020;8:2050312120918265. https://doi.org/10.1177/205031....
25.
Alberti KGMM, Zimmet P, Shaw J. Metabolic syndrome-a new world-wide definition. A consensus statement from the international diabetes federation. Diabetic Med. 2006;23(5):469–480. https://doi.org/10.1111/j.1464....
26.
Romero-Corral A, Somers VK, Sierra-Johnson J, et al. Accuracy of body mass index in diagnosing obesity in the adult general population. Int J Obes. 2008;32(6): 959–966. https://doi.org/10.1038/ijo.20....
27.
Kite C, Lahart IM, Afzal I, et al. Exercise, or exercise and diet for the management of polycystic ovary syndrome: a systematic review and meta-analysis. Syst Rev. 2019;8(1):51. https://doi.org/10.1186/s13643....
28.
Kim CH, Lee SH. Effectiveness of Lifestyle Modification in Polycystic Ovary Syndrome Patients with Obesity: A Systematic Review and Meta-Analysis. Life, 2022;12(2): 308. https://doi.org/10.3390/life12....
29.
Lim SS, Hutchison SK, Van Ryswyk E. et al. Lifestyle changes in women with polycystic ovary syndrome. Cochrane Database Syst Rev. 2019;3. https://doi.org/10.1002/146518....
30.
Mutsaerts M, Kuchenbecker W, Mol B, et al. Dropout is a problem in lifestyle intervention programmes for overweight and obese infertile women: a systematic review. Hum Reprod. 2013; 28(4):979–86. doi: 10.1093/humrep/det026.
31.
Ladson G, Dodson WC, Sweet SD, et al. The effects of metformin with lifestyle therapy in polycystic ovary syndrome: a randomized double-blind study. Fertil Steril. 2011; 95(8):2595-8.e1-6. doi: 10.1016/j.fertnstert.2011.05.048.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.