Online first
Current issue
Archive
Special Issues
About the Journal
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Board
Editorial Office
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
RESEARCH PAPER
Establishing score equivalence of the GDS-30 scale and International Classification of Functioning, Disability and Health range, using Rasch analysis
1
Institute of Medical Sciences, College of Medical Sciences of the University of Rzeszow, Poland
2
Institute of Health Sciences, College of Medical Sciences of the University of Rzeszow, Poland
3
Faculty of Medicine, Lazarski University, Warsaw, Poland
4
Department of Geriatrics, Neurosciences, Orthopedics, Center for Geriatric Medicine (CEMI), Institute of Internal Medicine
and Geriatrics, Catholic University of the Sacred Heart, Italy
5
Physical Medicine and Rehabilitation Unit, Department of Medical and Surgical Sciences, University of Catanzaro
“Magna Graecia”, Italy
Corresponding author
Agnieszka Beata Ćwirlej-Sozańska
Institute of Health Sciences, College of Medical Sciences of the University of Rzeszow, Warzywna 1a, 35-959, Rzeszow, Poland
Institute of Health Sciences, College of Medical Sciences of the University of Rzeszow, Warzywna 1a, 35-959, Rzeszow, Poland
Ann Agric Environ Med. 2023;30(1):105-110
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
Depression is a common problem among older adults. The Geriatric Depression Scale (GDS- 30) is a recommended tool for assessing the emotional state of the elderly. To-date, there are no data in literature on the description of GDS-30, according to the International Classification of Functioning, Disability and Health (ICF). The aim of the study is to transform the data obtained using the GDS-30 scale into the common scale of the ICF by applying the Rasch measurement theory.
Material and methods:
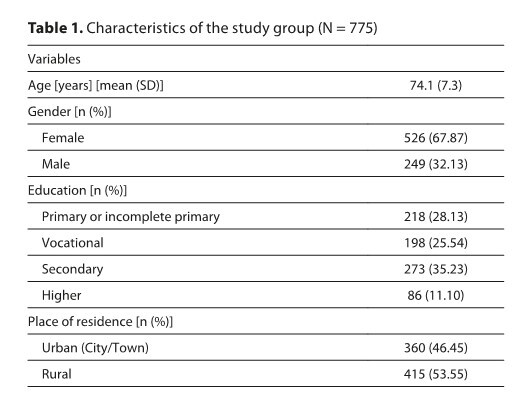
The study was conducted based on the results of 775 measurements made on people aged 65 and over. The Rasch model with the unconstrained Rasch parameter was used for the study.
Results:
The GDS-30 scale was transformed into the ICF scale, where 0 points on the ICF scale were assigned to 0 points on the GDS-30 scale, 1 on the ICF scale – 1–4 points on the GDS-30 scale, 2 on the ICF scale – 5–7 on the GDS-30, 3 on the ICF scale, and 8–19 points on the GDS-30, whereas 4 on the ICF scale, 20–30 points on the GDS-30.
Conclusions:
Taken together, the results showed that the GDS-30 scale can be reliably transferred to the universal ICF scale for the b152 Emotional functions code. The ability to transfer the results into the universal language of the ICF category provides a coding system for more efficient information management in health systems, allows for data aggregation, and offers the possibility to compare them. It is also invaluable for clinical practice and research, including creating meta-analyses.
Depression is a common problem among older adults. The Geriatric Depression Scale (GDS- 30) is a recommended tool for assessing the emotional state of the elderly. To-date, there are no data in literature on the description of GDS-30, according to the International Classification of Functioning, Disability and Health (ICF). The aim of the study is to transform the data obtained using the GDS-30 scale into the common scale of the ICF by applying the Rasch measurement theory.
Material and methods:
The study was conducted based on the results of 775 measurements made on people aged 65 and over. The Rasch model with the unconstrained Rasch parameter was used for the study.
Results:
The GDS-30 scale was transformed into the ICF scale, where 0 points on the ICF scale were assigned to 0 points on the GDS-30 scale, 1 on the ICF scale – 1–4 points on the GDS-30 scale, 2 on the ICF scale – 5–7 on the GDS-30, 3 on the ICF scale, and 8–19 points on the GDS-30, whereas 4 on the ICF scale, 20–30 points on the GDS-30.
Conclusions:
Taken together, the results showed that the GDS-30 scale can be reliably transferred to the universal ICF scale for the b152 Emotional functions code. The ability to transfer the results into the universal language of the ICF category provides a coding system for more efficient information management in health systems, allows for data aggregation, and offers the possibility to compare them. It is also invaluable for clinical practice and research, including creating meta-analyses.
REFERENCES (44)
1.
Malhi GS, Mann JJ. Depression. Lancet. 2018;392(10161):2299–2312. doi:10.1016/S0140-6736(18)31948-2.
2.
Haroz EE, Ritchey M, Bass JK, et al. How is depression experienced around the world? A systematic review of qualitative literature. Soc Sci Med. 2017;183:151–162. https://doi.org/10.1016/j.socs....
3.
WHO. Depression and other common mental disorders: global health estimates. World Health Organization, Geneva (2017).
4.
Maier A, Riedel-Heller SG, Pabst A, et al. Risk factors and protective factors of depression in older people 65+. A systematic review. PLoS One. 2021;16(5):e0251326. https://doi.org/10.1371/journa....
5.
Conde-Sala JL, Garre-Olmo J, Calvó-Perxas L, et al. Course of depressive symptoms and associated factors in people aged 65+ in Europe: A two-year follow-up. J Affect Disord. 2019;245:440–450. https://doi.org/10.1016/j.jad.....
6.
Zis P, Daskalaki A, Bountouni I, Sykioti P, et al. Depression and chronic pain in the elderly: links and management challenges. Clin Interv Aging. 2017;12:709–720. https://doi.org/ 10.2147/CIA.S113576.
7.
Ansari S, Anand A, Hossain B. Multimorbidity and depression among older adults in India: Mediating role of functional and behavioural health. PLoS One. 2022; 17(6):e0269646. https://doi.org/10.1371/journa....
8.
Lee GB, Kim HC, Jung SJ. Association between depression and disease-specific treatment. J Affect Disord. 2020;260:124–130. https://doi.org/10.1016/j.jad.....
9.
GBD 2016 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016 [published correction appears in Lancet. 2017 Oct 28;390(10106):e38]. Lancet. 2017;390(10100):1211–1259. https://doi.org/10.1016/S0140-....
10.
König H, König HH, Konnopka A. The excess costs of depression: a systematic review and meta-analysis. Epidemiol Psychiatr Sci. 2019; 29:e30. https://doi.org/10.1017/S20457....
11.
Conde-Sala JL, Garre-Olmo J, Calvó-Perxas L, et al. CAUSES, mortality rates and risk factors of death in community-dwelling Europeans aged 50 years and over: Results from the Survey of Health, Ageing and Retirement in Europe 2013–2015. Arch Gerontol Geriatr. 2020; 89:104035. https://doi.org/10.1016/j.arch... Form.
12.
Ghoneim MM, O’Hara MW. Depression and postoperative complications: an overview. BMC Surg. 2016; 16:5. https://doi.org/10.1186/s12893....
13.
World Health Organization. The mental health of older adults https://www.who.int/news-room/... (access: 26.05.2022).
14.
Oude Voshaar RC, Aprahamian I, Borges MK, et al. Excess mortality in depressive and anxiety disorders: The Lifelines Cohort Study. Eur Psychiatry. 2021;64(1):e54. https://doi.org/10.1192/j.eurp....
15.
Zenebe Y, Akele B, W/Selassie M, Necho M. Prevalence and determinants of depression among old age: a systematic review and meta-analysis. Ann Gen Psychiatry. 2021;20(1):55. https://doi.org/10.1186/s12991....
16.
COVID-19 Mental Disorders Collaborators. Global prevalence and burden of depressive and anxiety disorders in 204 countries and territories in 2020 due to the COVID-19 pandemic. Lancet. 2021; 398(10312):1700–1712. https://doi.org/10.1016/S0140-....
17.
Yesavage JA, Brink TL, Rose TL, Lum O, Huang V, Adey M, Leirer VO. Development and validation of a geriatric depression screening scale: A preliminary report. J. Psychiatr. Res. 1983;17:37–49.
18.
Nguyen TV, Nguyen KT, Nguyen PM, et al. Vietnamese Version of the Geriatric Depression Scale (30 Items): Translation, Cross-Cultural Adaptation, and Validation. Geriatrics (Basel). 2021;6(4):116. https://doi.org/10.3390/geriat....
19.
El-Den S, Chen TF, Gan YL, et al. The psychometric properties of depression screening tools in primary healthcare settings: A systematic review. J Affect Disord. 2018;225:503–522. https://doi.org/10.1016/j.jad.....
20.
Ballard ED, Yarrington JS, Farmer CA, et al. Parsing the heterogeneity of depression: An exploratory factor analysis across commonly used depression rating scales. J Affect Disord. 2018;231:51–57. https://doi.org/10.1016/j.jad.....
21.
Prodinger B, Tennant A, Stucki G. Standardized reporting of functioning information on ICF-based common metrics. Eur J Phys Rehabil Med. 2018;54(1):110–117. https://doi.org/10.23736/S1973....
22.
World Health Organization. International Classification of Functioning, Disability and Health (ICF). Geneva: WHO; 2001.
23.
Stucki G, Bickenbach J. Functioning: the third health indicator in the health system and the key indicator for rehabilitation. Eur J Phys Rehabil Med. 2017;53(1):134–138. https://doi.org/10.23736/S1973....
24.
Gimigliano F, de Sire A, Gastaldo M, et al. SIMFER Residents Section Group. Use of the International Classification of Functioning, Disability and Health Generic-30 Set for the characterization of outpatients: Italian Society of Physical and Rehabilitative Medicine Residents Section Project. Eur J Phys Rehabil Med. 2019;55(2):258–264. https://doi.org/10.23736/S1973....
25.
Christensen KB, Kreiner S, Mesbah M. Rasch Models in Health. John Wiley & Sons; 2013.
26.
Hobart J, Cano S. Improving the evaluation of therapeutic interventions in multiple sclerosis: the role of new psychometric methods. Health Technol Assess. 2009;13(12):iii-177. https://doi.org/10.3310/hta131....
27.
Rash G. Probabilistic Models for Some Intelligence and Attainment Tests. Copenhagen: Danish Institute for Educational Research; 1960.
28.
Stucki G, Bickenbach J, Melvin J. Strengthening Rehabilitation in Health Systems Worldwide by Integrating Information on Functioning in National Health Information Systems. Am J Phys Med Rehabil. 2017;96(9):677–681. https://doi.org/10.1097/PHM.00....
29.
World Health Organization. Rehabilitation in health systems: guide for action https://www.who.int/publicatio... (access: 26.05.2022).
30.
Główny Urząd Statystyczny. Sytuacja demograficzna Polski do 2020 roku. Zgony i umieralność https://stat.gov.pl/obszary-te... (access: 26.05.2022).
31.
Piotrowicz K, Romanik W, Skalska A, et al. The comparison of the 1972 Hodkinson’s Abbreviated Mental Test Score (AMTS) and its variants in screening for cognitive impairment. Aging Clin Exp Res. 2019;31(4):561–566. https://doi.org/10.1007/s40520....
32.
Huang F, Wang H, Wang Z, et al. Is geriatria depression scale a valid instrument to screen depression in Chinese community-dwelling elderly?. BMC Geriatr. 2021;21(1):310. https://doi.org/10.1186/s12877....
33.
Albiński R, Kleszczewska-Albińska A, Bedyńska S. Geriatryczna Skala Depresji (GDS). Trafność i rzetelność róznych wersji tego narzedzia-przeglad badań [Geriatric Depression Scale (GDS). Validity and reliability of different versions of the scale-review]. Psychiatr Pol. 2011;45(4):555–562.
34.
Cieza A, Fayed N, Bickenbach J, et al. Refinements of the ICF Linking Rules to strengthen their potential for establishing comparability of health information. Disabil Rehabil. 2019;41(5):574–583. https://doi.org/10.3109/096382....
35.
R Core Team. R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria, 2020. URL https://www.R-project.org/.
36.
Grimby G, Tennant A, Tesio L. The use of raw scores from ordinal scales: time to end malpractice? J Rehabil Med. 2012;44(2):97–98. https://doi.org/10.2340/165019....
37.
Brzezińska J. Irt and Rasch Models in test measurement. Research Papers of Wrocław University of Economics Copyright by Uniwersytet Ekonomiczny we Wrocławiu. Wrocław; 2016.
38.
Vanbellingen T, Ottiger B, Pflugshaupt T, et al. The Responsiveness of the Lucerne ICF-Based Multidisciplinary Observation Scale: A Comparison with the Functional Independence Measure and the Barthel Index. Front Neurol. 2016;7:152. https://doi.org/10.3389/fneur.....
39.
Ģiga L, Pētersone A, Čakstiņa S, et al. Comparison of content and psychometric properties for assessment tools used for brain tumor patients: a scoping review. Health Qual Life Outcomes. 2021;19(1):234. https://doi.org/10.1186/s12955....
40.
Noonan VK, Kopec JA, Noreau L, et al. Comparing the content of participation instruments using the international classification of functioning, disability and health. Health Qual Life Outcomes. 2009; 7:93. https://doi.org/10.1186/1477-7....
41.
Galli T, Mirata P, Foglia E, et al. A comparison between WHODAS 2.0 and Modified Barthel Index: which tool is more suitable for assessing the disability and the recovery rate in orthopedic rehabilitation? Clinicoecon Outcomes Res. 2018;10:301–307. https://doi.org/ 10.2147/CEOR.S150526.
42.
Tesio L. Measuring behaviours and perceptions: Rasch analysis as a tool for rehabilitation research [published correction appears in J Rehabil Med. 2003 Nov;35(6):294]. J Rehabil Med. 2003; 35(3):105–115. https://doi.org/10.1080/165019....
43.
Andrich D. Rating scales and Rasch measurement. Expert Rev Pharmacoecon Outcomes Res. 2011;11(5):571–585. https://doi.org/10.1586/erp.11....
44.
Reise SP, Haviland MG. Item response theory and the measurement of clinical change. J Pers Assess. 2005;84(3):228–238. https://doi.org/10.1207/s15327....
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.