Online first
Current issue
Archive
Special Issues
About the Journal
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Board
Editorial Office
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
RESEARCH PAPER
Clinical and electroencephalographic characteristics of febrile seizures – a retrospective cohort study
1
Department of Paediatric Neurology, Medical University, Warsaw, Poland
2
Department of Paediatric Neurosurgery, Bogdanowicz Memorial Hospital for Children, Warsaw, Poland
3
Department of Descriptive and Clinical Anatomy, Medical University, Warsaw, Poland
Corresponding author
Tymon Skadorwa
Department of Peadiatric Neurosurgery, Bogdanowicz Memorial Hospital for Children, Nieklanska 4/24, 03-924 Warsaw, Poland
Department of Peadiatric Neurosurgery, Bogdanowicz Memorial Hospital for Children, Nieklanska 4/24, 03-924 Warsaw, Poland
Ann Agric Environ Med. 2022;29(3):401-406
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
Febrile seizures (FS) are the most common type of seizures in childhood. Depending on focality, duration and possible recurrence FS are divided into simple (SFS), complex (CFS) and simple plus (SFS+). Simple FS are considered not to require detailed diagnostics nor electroencephalographic (EEG) studies, even though some cases present EEG abnormalities that may affect the initial diagnosis and long-term prognosis. The aim of the study was to assess the usefulness of EEG as a potential prognostic neuromarker of FS.
Material and methods:
103 FS children aged 5–55 months (SFS – 62 cases (60%); SFS+ – 15 cases (15%); CFS – 26 cases (25%) were retrospectively analyzed. EEG was performed in all cases after the resolution of fever (3rd-7th day). The clinical characteristics (seizure morphology, episode duration and recurrence) were confronted with EEG findings (normal vs. epileptiform pattern: generalized or focal). The results were analyzed statistically to look for prognostically useful correlations.
Results:
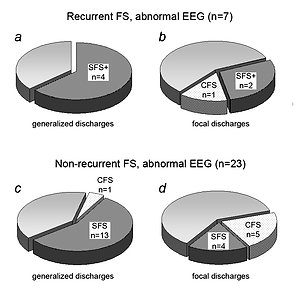
Abnormal EEG pattern was recorded in 29% of patients (SFS 27%; SFS+ 40%; CFS 27%). Generalized epileptiform discharges were noted in 18 cases (SFS 21%; SFS+ 27%; CFS 4%) while focal EEG discharges were seen in 12 cases (SFS 6%; SFS+ 13%; CFS 23%). Generalized FS in 30% were associated with generalized (19%) or focal (11%) EEG discharges.
Conclusions:
The current protocol of FS management does not warrant further diagnostics in 27–40% of FS children with abnormal EEG. SFS+ children are be the most underdiagnosed group, with a greater number of EEG abnormalities compared to SFS and CFS. It seems reasonable to extend the routine EEG diagnostics into this group of FS patients.
Febrile seizures (FS) are the most common type of seizures in childhood. Depending on focality, duration and possible recurrence FS are divided into simple (SFS), complex (CFS) and simple plus (SFS+). Simple FS are considered not to require detailed diagnostics nor electroencephalographic (EEG) studies, even though some cases present EEG abnormalities that may affect the initial diagnosis and long-term prognosis. The aim of the study was to assess the usefulness of EEG as a potential prognostic neuromarker of FS.
Material and methods:
103 FS children aged 5–55 months (SFS – 62 cases (60%); SFS+ – 15 cases (15%); CFS – 26 cases (25%) were retrospectively analyzed. EEG was performed in all cases after the resolution of fever (3rd-7th day). The clinical characteristics (seizure morphology, episode duration and recurrence) were confronted with EEG findings (normal vs. epileptiform pattern: generalized or focal). The results were analyzed statistically to look for prognostically useful correlations.
Results:
Abnormal EEG pattern was recorded in 29% of patients (SFS 27%; SFS+ 40%; CFS 27%). Generalized epileptiform discharges were noted in 18 cases (SFS 21%; SFS+ 27%; CFS 4%) while focal EEG discharges were seen in 12 cases (SFS 6%; SFS+ 13%; CFS 23%). Generalized FS in 30% were associated with generalized (19%) or focal (11%) EEG discharges.
Conclusions:
The current protocol of FS management does not warrant further diagnostics in 27–40% of FS children with abnormal EEG. SFS+ children are be the most underdiagnosed group, with a greater number of EEG abnormalities compared to SFS and CFS. It seems reasonable to extend the routine EEG diagnostics into this group of FS patients.
ACKNOWLEDGEMENTS
The authors would like to acknowledge Dr. Adam Zieliński and Dr. Małgorzata Paciorkowska from Bogdanowicz Memorial Hospital for Children, Warsaw, who contributed to the collection of clinical data.
REFERENCES (40)
1.
Leung AK, Hon KL, Leung TN. Febrile seizures: An overview. Drugs Context. 2018; 7: 1–12. https://doi.org/10.7573/dic.21....
2.
Harini C, Nagarajan E, Kimia AA, et al. Utility of initial EEG in first complex febrile seizure. Epilepsy Behav. 2015; 52: 200–204. https://doi.org/10.1016/j.yebe....
3.
Gupta A. Febrile seizures. Continuum (Minneap Minn). 2016; 22(1): 51–59. https://doi.org/10.1212/CON.00....
4.
Hesdorffer DC, Shinnar S, Lax DN, et al. Risk factors for subsequent febrile seizures in the FEBSTAT study. Epilepsia. 2016; 57(7): 1042–1047. https://doi.org/10.1111/epi.13....
5.
Cross JH. Fever and fever-related epilepsies. Epilepsia. 2012; 53: 3–8. https://doi.org/10.1111/j.1528....
6.
Mastrangelo M, Midulla F, Moretti C. Actual insights into the clinical management of febrile seizures. Eur J Pediatr. 2014; 173(8): 977–982. https://doi.org/10.1007/s00431....
7.
Ma QL, Wang B, Chen GF, et al. Association between SCN1A rs3812718 polymorphism and generalized epilepsy with febrile seizures plus. Zhongguo Dang Dai Er Ke Za Zhi. 2018; 20(2): 130–133. https://doi.org/10.7499/j.issn....
8.
Ma H, Guo Y, Chen Z, et al. Mutations in the sodium channel genes SCN1A, SCN3A, and SCN9A in children with epilepsy with febrile seizures plus (EFS+). Seizure. 2021; 88: 146–152. https://doi.org/10.1016/J.SEIZ....
9.
Fox K, Wells ME, Tennison M, et al. Febrile Infection-Related Epilepsy Syndrome (FIRES): A Literature Review and Case Study. Neurodiagn J. 2017; 57(3): 224–233. https://doi.org/10.1080/216468....
10.
Culleton S, Talenti G, Kaliakatsos M, et al. The spectrum of neuroimaging findings in febrile infection-related epilepsy syndrome (FIRES): A literature review. Epilepsia. 2019; 60(4): 585–592. https://doi.org/10.1111/epi.14....
11.
Cappellari AM, Brizio C, Mazzoni MB, et al. Predictive value of EEG for febrile seizure recurrence. Brain Dev. 2018; 40(4): 311–315. https://doi.org/10.1016/j.brai.... 2017.12.004.
12.
Wilmshurst JM, Gaillard WD, Vinayan KP, et al. Summary of recommendations for the management of infantile seizures: Task Force Report for the ILAE Commission of Pediatrics. Epilepsia. 2015; 56(8): 1185–1197. https://doi.org/10.1111/epi.13....
13.
Kannikeswaran N, Sivaswamy L, Farooqi A, et al. Children With Complex Febrile Seizures: Is Hospital Admission Necessary? Clin Pediatr (Phila). 2021; 60(8): 363–369. https://doi.org/10.1177/000992....
14.
Kubota J, Higurashi N, Hirano D, et al. Body temperature predicts recurrent febrile seizures in the same febrile illness. Brain Dev. 2021; 43(7): 768–774. https://doi.org/10.1016/J.BRAI....
15.
Offringa M, Newton R, Nevitt SJ, et al. Prophylactic drug management for febrile seizures in children. Cochrane Database Syst Rev. 2021; 6(6) https://doi.org/10.1002/146518....
16.
Patel N, Ram D, Swiderska N, et al. Febrile seizures. BMJ. 2015; 351: h4240. https://doi.org/10.1136/bmj.h4....
17.
Patterson JL, Carapetian SA, Hageman JR, et al. Febrile seizures. Pediatr Ann. 2013; 42(12): e258–e263. https://doi.org/10.3928/009044....
18.
Jain A, Tiwari S, Padickaparambil S. Cross-disciplinary appraisal of knowledge and beliefs regarding the diagnosis of autism spectrum disorders in India: A cross-sectional survey. Indian J Psychol Med. 2020; 42(3): 219–224. https://doi.org/10.4103/IJPSYM....
19.
Gencpinar P, Yavuz H, Bozkurt Ö, et al. The risk of subsequent epilepsy in children with febrile seizure after 5 years of age. Seizure. 2017; 53: 62–65. https://doi.org/10.1016/j.seiz....
20.
Kim H, Byun SH, Kim JS, et al. Clinical and EEG risk factors for subsequent epilepsy in patients with complex febrile seizures. Epilepsy Res. 2013; 105(1–2): 158–163. https://doi.org/10.1016/j.eple....
21.
Hwang G, Kang H, Park SY, et al. Predictors of unprovoked seizure after febrile seizure: short-term outcomes. Brain Dev. 2015; 37(3); 315–321. https://doi.org/10.1016/J.BRAI....
22.
Klotz KA, Özcan J, Sag Y, et al. Anxiety of families after first unprovoked or first febrile seizure – A prospective, randomized pilot study. Epilepsy Behav. 2021; 122. https://doi.org/10.1016/J.YEBE....
23.
Mirski A, Pachalska M, Mirska N, et al. An evaluation of personalized neurofeedback training for rolandic epilepsy: a case study. Acta Neuropsychologica 2014; 12(3): 271–287. https://doi.org/10.13140/2.1.4....
24.
Kropotov JD. Functional neuromarkers for neuropsychology. Acta Neuropsychologica 2018; 16(1): 1–7. https://doi.org/10.5604/01.300....
25.
Thébault-Dagher F, Deguire F, Knoth IS, et al. Prolonged and unprolonged complex febrile seizures differently affect frontal theta brain activity. Epilepsy Res. 2020; 159: 106217. https://doi.org/10.1016/j.eple....
26.
Billstedt E, Nilsson, G, Leffler L, et al. Cognitive functioning in a representative cohort of preschool children with febrile seizures. Acta Paediatr. 2020; 109(5): 989–994. https://doi:10.1111/apa.15059.
27.
Gradisnik P, Zagradisnik B, Palfy M, et al. Predictive value of paroxysmal EEG abnormalities for future epilepsy in focal febrile seizures. Brain Dev. 2015; 37(9): 868–873. https://doi.org/10.1016/j.brai....
28.
Duffner PK, Berman PH, Baumann RJ, et al. Clinical practice guideline – Neurodiagnostic evaluation of the child with a simple febrile seizure. Pediatrics. 2011; 127(2): 389–394. https://doi.org/10.1542/peds.2....
29.
Lee SH, Byeon JH, Kim GH, et al. Epilepsy in children with a history of febrile seizures. Korean J Pediatr. 2016; 59(2): 74–79. https://doi.org/10.3345/kjp.20....
30.
Seinfeld SA, Pellock JM, Kjeldsen MJ, et al. Epilepsy after Febrile Seizures: Twins Suggest Genetic Influence. Pediatr Neurol. 2016; 55: 14–16. https://doi.org/10.1016/j.pedi....
31.
Tsai JD, Mou CH, Chang HY, et al. Trend of subsequent epilepsy in children with recurrent febrile seizures: A retrospective matched cohort study. Seizure. 2018; 61: 164–169. https://doi.org/10.1016/j.seiz....
32.
Laino D, Mencaroni E, Esposito S. Management of pediatric febrile seizures. Int J Environ Res Public Health. 2018; 15(10): 2232. https://doi.org/10.3390/ijerph....
33.
Shah PB, James S, Elayaraja S. EEG for children with complex febrile seizures. Cochrane Database Syst Rev. 2020; 4(4): 1–23. https://doi.org/10.1002/146518....
34.
Pavlidou E, Panteliadis C. Prognostic factors for subsequent epilepsy in children with febrile seizures. Epilepsia. 2013; 54(12): 2101–2107. https://doi.org/10.1111/epi.12....
35.
Natsume J, Hamano SI, Iyoda K, et al. New guidelines for management of febrile seizures in Japan. Brain Dev. 2017; 39(1): 2–9. https://doi.org/10.1016/j.brai....
36.
Prosad S. Management of febrile convulsion in children. Emerg Nurse. 2015; 23(2): 18–25. https://doi.org/10.7748/en.23.....
37.
Sooyoung L. Electroencephalographic Approach for Early Diagnosis of Acute Encephalopathy and Encephalitis. Hideo Yamanouchi, Solomon L. Moshé, Akihisa Okumura, editors. Acute Encephalopathy and Encephalitis in Infancy and Its Related Disorders. Elsevier; 2018. p. 71–76.
38.
Oguri M, Saito Y, Fukuda C, et al. Distinguishing Acute Encephalopathy with Biphasic Seizures and Late Reduced Diffusion from Prolonged Febrile Seizures by Acute Phase EEG Spectrum Analysis. Yonago Acta Med. 2016; 59(1): 1–14.
39.
Tashkandi M, Baarma D, Tricco AC, et al. EEG of asymptomatic first-degree relatives of patients with juvenile myoclonic, childhood absence and rolandic epilepsy: a systematic review and meta-analysis. Epileptic Disord. 2019; 21(1): 30–41. https://doi.org/10.1684/epd.20....
40.
Jeong KA, Han MH, Lee EH, et al. Early postictal electroencephalography and correlation with clinical findings in children with febrile seizures. Korean J Pediatr. 2013; 56(12): 534–539. https://doi.org/10.3345/kjp.20....
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.