Online first
Current issue
Archive
Special Issues
About the Journal
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Board
Editorial Office
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
RESEARCH PAPER
Patient satisfaction with oncological care during the virus pandemic – SARS-CoV-2 taking into account social and demographic factors
1
Jan Grodek State University in Sanok, Poland
2
Collegium Medicum, Faculty of Medicine, Cardinal Stefan Wyszyński University, Warsaw, Poland
3
Department of Public Health, Medical University, Wrocław, Poland
4
Faculty of Health Sciences, Calisia University, Kalisz, Poland
Corresponding author
Ann Agric Environ Med. 2023;30(1):135-141
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
The aim of the study was to examine the perception of medical services by oncological patients during the pandemic, identifying the key factors influencing it. The assessment of patient satisfaction with the treatment and care provided by doctors and other hospital staff provides important information on the quality of health services.
Material and methods:
The study involved 394 patients diagnosed with cancer treated as inpatients in five oncology departments. The diagnostic survey method was used with a proprietary questionnaire and the standardized EORTC IN-PATSAT32 questionnaire. Calculations were carried out using Statistica 10.0 with p≤0.05 s considered statistically significant.
Results:
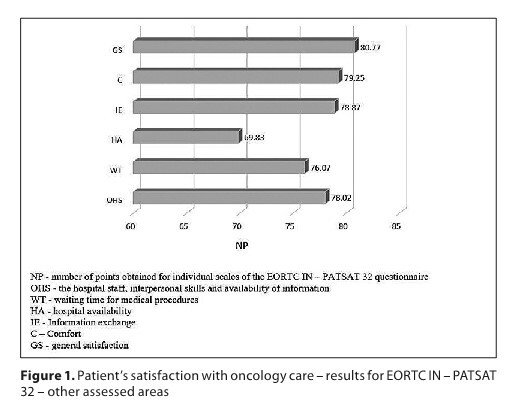
Overall patient satisfaction with cancer care was 80.77/100. Higher values were shown for the competences of nurses than for doctors, especially for their interpersonal skills (79.34 – nurses vs. 74.13 – doctors) and availability (80.11 – nurses vs. 75.6 – doctors). It was also shown that the level of satisfaction with cancer care increased with age; women rated cancer care lower than men (p = 0.031), particularly its aspect related to the competences of doctors. A lower degree of satisfaction was observed among rural residents (p=0.042). Other demographic data, such as marital status and education, determined satisfaction with cancer care on the selected scale although it did not affect the overall level of satisfaction.
Conclusions:
The analysed socio-demographic factors, primarily age, gender and place of residence, determined some of the scales concerning patient satisfaction with cancer care during the COVID-19 pandemic. The results of this and other studies of a similar profile should be used in the formation of health policy, particularly in implementing programmes to improve the quality of cancer care in Poland.
The aim of the study was to examine the perception of medical services by oncological patients during the pandemic, identifying the key factors influencing it. The assessment of patient satisfaction with the treatment and care provided by doctors and other hospital staff provides important information on the quality of health services.
Material and methods:
The study involved 394 patients diagnosed with cancer treated as inpatients in five oncology departments. The diagnostic survey method was used with a proprietary questionnaire and the standardized EORTC IN-PATSAT32 questionnaire. Calculations were carried out using Statistica 10.0 with p≤0.05 s considered statistically significant.
Results:
Overall patient satisfaction with cancer care was 80.77/100. Higher values were shown for the competences of nurses than for doctors, especially for their interpersonal skills (79.34 – nurses vs. 74.13 – doctors) and availability (80.11 – nurses vs. 75.6 – doctors). It was also shown that the level of satisfaction with cancer care increased with age; women rated cancer care lower than men (p = 0.031), particularly its aspect related to the competences of doctors. A lower degree of satisfaction was observed among rural residents (p=0.042). Other demographic data, such as marital status and education, determined satisfaction with cancer care on the selected scale although it did not affect the overall level of satisfaction.
Conclusions:
The analysed socio-demographic factors, primarily age, gender and place of residence, determined some of the scales concerning patient satisfaction with cancer care during the COVID-19 pandemic. The results of this and other studies of a similar profile should be used in the formation of health policy, particularly in implementing programmes to improve the quality of cancer care in Poland.
REFERENCES (31)
1.
Sung H, Ferlay J, Siegel RL, et al. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J Clin. 2021;71(3):209–249. https://doi.org/10.3322/caac.2....
3.
Miljanović M, Sindik J, Milunović V, et al. Psychosocial Determinants of Satisfaction with Hospital Care in Adult Patients Suffering from Advanced Cancer. Acta Clin Croat. 2017;56(2):218–226. https://doi.org/10.20471/acc.2....
4.
Vosburg RW, Robinson KA. Telemedicine in primary care during the COVID-19 pandemic: provider and patient satisfaction examined. Telemed J E Health. 2022;28(2):167–175. https://doi.org/10.1089/tmj.20....
5.
Grodecka-Gazdecka S, Zaborek P, Didkowska J, et al. System-related delays in diagnosis and treatment of breast cancer in Poland. Nowotwory. J Oncol. 2014;64(6):483–490.
6.
Osowiecka K, Rucinska M, Nowakowski JJ, et al. How Long Are Cancer Patients Waiting for Oncological Therapy in Poland? Int J Environ Res Public Health. 2018;15(4):577. https://doi.org/10.3390/ijerph....
7.
Konieczny M, Cipora E, Roczniak W, et al. Impact of Time to Initiation of Treatment on the Quality of Life of Women with Breast Cancer. Int J Environ Res Public Health. 2020;17(22):8325. https://doi.org/10.3390/ijerph....
8.
Indini A, Aschele C, Cavanna L, et al. Reorganisation of medical oncology departments during the novel coronavirus disease-19 pandemic: a nationwide Italian survey. Eur J Cancer. 2020;132:17–23. https://doi.org/10.1016/j.ejca....
9.
Trapani D, Marra A, Curigliano G. The experience on coronavirus disease 2019 and cancer from an oncology hub institution in Milan, Lombardy Region. Eur J Cancer. 2020;132:199–206. https://doi.org/:10.1016/j.ejc....
10.
Hays RD, Samuel SA. Patient experience with in-person and telehealth visits before and during the COVID-19 pandemic at a large integrated health system in the United States. J Gen Intern Med. 2022;37(4):847–852. https://doi.org/10.1007/s11606....
11.
Wadasadawala T, Mangaj A, Mokal S, et al. Measuring Satisfaction in Breast Cancer Patients Receiving Ambulatory Care: A Validation Study. Indian J Med Paediatr Oncol. 2021;10:464–473. https://doi.org/:10.1055/s-004....
12.
Pishkuhi MA, Salmaniyan S, Nedjat S, et al. Psychometric properties of the Persian version of satisfaction with care EORTC-in-patsat32 questionnaire among Iranian cancer patients. Asian Pac J Cancer Prev. 2014;15(23):10121–8. https://doi.org/:10.7314/.
13.
Obročníková A, Majerníková L. Patient satisfaction with health care in an oncology setting. Pielegniarstwo XXI wieku / Nursing in the 21st Century. 2017;15:20–24. https://doi.org/:10.1515/pielx....
14.
Tsilika E, Parpa E, Galanopoulou A, et al. The effect of cancer patients’ attachment orientations on their satisfaction of medical care. J BUON. 2019;24(4):1712–1718.
15.
Groff SL, Carlson LE, Tsang K, et al. Cancer patients’ satisfaction with care in traditional and innovative ambulatory oncology clinics. J Nurs Care Qual. 2008;23(3):251–257. https://doi.org/:10.1097/01.NC....
16.
Costantini A, Grassi L, Picardi A, et al. Awareness of cancer, satisfaction with care, emotional distress, and adjustment to illness: an Italian multicenter study. Psychooncology. 2015;24(9):1088–96. https://doi.org/: 10.1002/pon.3768.
17.
Brédart A, Bottomley A, Blazeby JM, et al. An international prospective study of the EORTC cancer in-patient satisfaction with care measure (EORTC IN-PATSAT32). Eur J Cancer. 2005;41(14):2120–2131. https://doi.org/:10.1016/j.ejc....
18.
Bos-van den Hoek DW, Visser LNC, Brown RF, et al. Communication skills training for healthcare professionals in oncology over the past decade: a systematic review of reviews. Curr Opin Support Palliat Care. 2019;13(1)33–45. https://doi.org/10.1097/SPC.00....
19.
Thornton RH, Dauer LT, Shuk E, et al. Patient perspectives and preferences for communication of medical imaging risks in a cancer care setting. Radiology. 2015;275(2):545–552. https://doi.org/10.1148/radiol....
20.
Al-Quteimat OM, Amer AM. The Impact of the COVID-19 Pandemic on Cancer Patients. Am J Clin Oncol. 2020;43(6):452–455. https://doi.org/10.1097/COC.00....
21.
Cohen M, Yagil D, Aviv A, et al. Cancer patients attending treatment during COVID-19: intolerance of uncertainty and psychological distress. J Cancer Surviv. 2022;16:1478–1488. https://doi.org/10.1007/s11764....
22.
de Joode K, Dumoulin DW, Engelen V, et al. Impact of the coronavirus disease 2019 pandemic on cancer treatment: the patients’ perspective. Eur J Cancer. 2020;136:132–139. https://doi.org/:10.1016/j.ejc....
23.
Zadnik V, Mihor A, Tomsic S, et al. Impact of COVID-19 on cancer diagnosis and management in Slovenia – preliminary results. Radiol Oncol. 2020;54(3):329–334. https://doi.org/:10.2478/raon-....
24.
Akhbari F, Hosseini M, Arab M, et al. Study of effective factors on inpatient satisfaction in Hospitals of Tehran University of medical science. Sci J School Public Health Instit Public Health Res. 2006;4(3):25–36.
25.
Hajifathali A, Ainy A, Jafari H, et al. In-patient satisfaction and its related factors in Taleghani University hospital, Tehran, Iran. Pak J Med Sci. 2008;24(2):274–277.
26.
Sherlaw-Johnson C, Datta P, McCarthy M. Hospital differences in patient satisfaction with care for breast, colorectal, lung and prostate cancers. Eur J Cancer. 2008;44(11):1559–65. https://doi.org/:10.1016/j.ejc....
27.
Fallowfield LJ. Treatment decision-making in breast cancer: the patient-doctor relationship. Breast Cancer Res Treat. 2008;112:5–13. https://doi.org/:10.1007/s1054....
28.
Djordjevic I, Vasiljevic D. The Effect of Sociodemographic Factors on the Patient Satisfaction with Health Care System. Ser J Exp Clin Res. 2019;20(3):251–255. https://doi.org/10.1515/sjecr-....
29.
Alosaimi FD, Alsaleh FS, Alsughayer LY, et al. Psychosocial and clinical predictors of patient satisfaction with cancer care. Saudi Pharm J. 2022;30(4):414–420. https://doi.org/:10.1016/j.jsp....
30.
Moreno PI, Ramirez AG, San Miguel-Majors SL, et al. Satisfaction with cancer care, self-efficacy, and health-related quality of life in Latino cancer survivors. Cancer. 2018;124(8):1770–1779. https://doi.org/:10.1002/cncr.....
31.
Chino F, Peppercorn J, Taylor DH Jr, et al. Self-reported financial burden and satisfaction with care among patients with cancer. Oncologist. 2014;19(4):414–420. https://doi.org/10.1634/theonc....
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.