Online first
Current issue
Archive
Special Issues
About the Journal
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Board
Editorial Office
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
RESEARCH PAPER
Opinions of citizens of the Czech Republic on the role of nurses in primary care during the COVID-19 pandemic
1
Faculty of Health and Social Sciences, Institute of Nursing, Midwifery and Emergency Care, University of South Bohemia, České Budějovice, Czech Republic
2
Faculty of Health and Social Sciences, Institute of Humanities in Helping Professions, University of South Bohemia,
České Budějovice, Czech Republic
3
Faculty of Health and Social Sciences, Institute of Nursing, Midwifery and Emergency Care, Hospital, Infectious Disease
Department, University of South Bohemia, České Budějovice, Czech Republic
4
Faculty of Health and Social Sciences, Institute of Laboratory Diagnostics and Public Health, University of South
Bohemia, České Budějovice, Czech Republic
Corresponding author
Sylva Bartlova
University of South Bohemia in České Budějovice, Faculty of Health and Social Sciences, Institute of Nursing, Midwifery and Emergency Care, J .Boreckeho 1167/27, 370 11, České Budějovice, Czech Republic
University of South Bohemia in České Budějovice, Faculty of Health and Social Sciences, Institute of Nursing, Midwifery and Emergency Care, J .Boreckeho 1167/27, 370 11, České Budějovice, Czech Republic
Ann Agric Environ Med. 2023;30(1):164-170
Limitations of the study. For the calculation of the sample
size, a confidence level of 99% and confidence interval or
margin of error of 3 % were established.
Ethical approval. The study was conducted per ethical
principles and approved by the relevant Ethics Committee
(No.004/2020, dated 15 June 2020).
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
In spite of the general current decrease in COVID-19 incidence, the epidemiological situation on the territory of the Czech Republic is still unfavourable. Nurses play an essential role in the fight against this disease.
Material and methods:
A non-standardized questionnaire was used to discover the expectations regarding nursing care provided during the COVID-19 pandemic. The sample of respondents was constructed using quota selection. The sample consisted of 1,815 respondents.
Results:
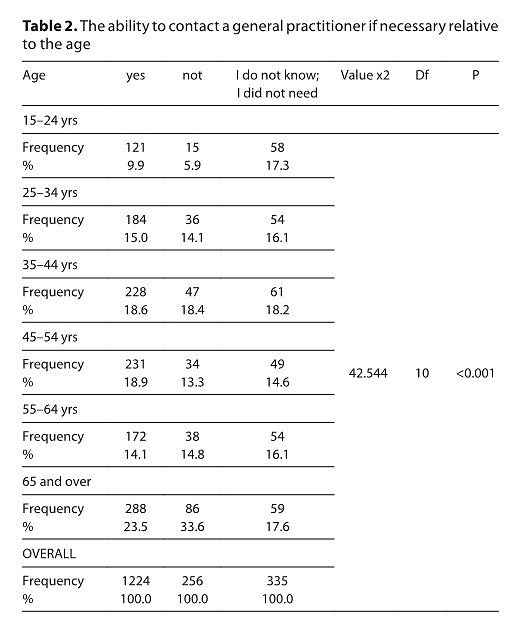
The study identified a significant correlation between the age of respondents and the method used to contact general practitioners (p < 0.001). The oldest respondents (65+) more likely contacted GPs by phone. Respondents with basic education used outpatient services more often before than during the pandemic (p < 0.05). The behaviour of nurses was considered as professional and accommodating. The oldest respondents (65+) reported nurses did not to make them feel rushed. Other age groups rated nurses more critically (p < 0.01). Respondents, especially women, described the psychological burden on nurses during the COVID-19 pandemic as demanding (p < 0.01). Women, more than men, reported that nurses lacked protective equipment during the pandemic (p < 0.05). The use of an online system was significantly influenced by respondent education (p 0.001). Respondents with lower education were less likely to welcome this option.
Conclusions:
Due to the persisting COVID-19 incidence on the territory of the Czech Republic, citizens` opinions of the position of nurse in primary care in the period of COVID- 19 pandemics need to be known.The behaviour of nurses was considered to be accommodating and satisfactory.
In spite of the general current decrease in COVID-19 incidence, the epidemiological situation on the territory of the Czech Republic is still unfavourable. Nurses play an essential role in the fight against this disease.
Material and methods:
A non-standardized questionnaire was used to discover the expectations regarding nursing care provided during the COVID-19 pandemic. The sample of respondents was constructed using quota selection. The sample consisted of 1,815 respondents.
Results:
The study identified a significant correlation between the age of respondents and the method used to contact general practitioners (p < 0.001). The oldest respondents (65+) more likely contacted GPs by phone. Respondents with basic education used outpatient services more often before than during the pandemic (p < 0.05). The behaviour of nurses was considered as professional and accommodating. The oldest respondents (65+) reported nurses did not to make them feel rushed. Other age groups rated nurses more critically (p < 0.01). Respondents, especially women, described the psychological burden on nurses during the COVID-19 pandemic as demanding (p < 0.01). Women, more than men, reported that nurses lacked protective equipment during the pandemic (p < 0.05). The use of an online system was significantly influenced by respondent education (p 0.001). Respondents with lower education were less likely to welcome this option.
Conclusions:
Due to the persisting COVID-19 incidence on the territory of the Czech Republic, citizens` opinions of the position of nurse in primary care in the period of COVID- 19 pandemics need to be known.The behaviour of nurses was considered to be accommodating and satisfactory.
ACKNOWLEDGEMENTS
The study was supported by the Ministry of Health of the Czech Republic, Grant No. NU 21-09-00300.
REFERENCES (30)
1.
Labrague LJ, De Los Santos JAA. COVID-19 anxiety among front-line nurses: Predictive role of organisational support, personal resilience and social support. J Nurs Manag. 2020;28(7):1653–1661. https://doi.org/10.1111/jonm.1....
2.
Šupíková M, Jankovičová J, Jarabicová O, et al. Factors affecting nurses’ mental health during the COVID-19 pandemic. Kontakt. 2022;24(3):205–201. https://doi.org/10.32725/kont.....
3.
Aragones E, del Cura-González I, Hernández-Rivas L, et al. Psychological impact of the COVID-19 pandemic on primary care workers: a cross-sectional study. Br J Gen Pract. 2022;72(720):e501–e510. https://doi.org/10.3399/BJGP.2....
4.
Díaz-Agea JL, Orcajada-Munoz I, Leal-Costa C, et al. How Did the Pandemic Affect Communication in Clinical Settings? A Qualitative Study with Critical and Emergency Care Nurses. Healthcare (Basel). 2022;10(2):373. https://doi.org/10.3390/health....
5.
Sharma R, Vishwas AS, Jelly P. Impact of COVID-19: nursing perspective and concern. Int J Community Med Public Health. 2022;7(11):4648–4652. https://doi.org/10.3390/health....
6.
Subbiah N, Jeganathan A. Challenges Faced by the Nursing Professionals in Management of Patients with COVID-19. Int J Community Health Nurs. 2021;4(1). https://doi.org/10.37628/IJCHN.
7.
Wittenberg E, Goldsmith JV, Chen C, et al. Opportunities to improve COVID-19 provider communication resources: A systematic review. Patient Educ Couns. 2021;104(3):438–451. https://doi.org/10.1016/j.pec.....
8.
Diogo P, Lemos,O, Rodriques J. The frontline nurses’challenges fighting against COVID-19: Nursing emotional labour performance. 24th International Nursing Research Conference, 2020 Nov 9–13; Pamplona, Spain. https://doi.org/10.13140/RG.2.....
9.
WHO a. State of the world’s nursing 2020: investing in education, jobs and leadership. Geneva World Health organization, 2020.
10.
Pospíšilová M. Dopad pandemie na ženy ve zdravotnictví. 2021 Sociologický ústav AV ČR. https://www.soc.cas.cz/aktuali... zeny-ve zdravotnictvi (access: 2021.12.26).
11.
Verhoeven V, Tsakitzidis G, Philips H, et al. Impact of the COVID-19 pandemic on the core functions of primary care: will the cure be worse than the disease? A qualitative interview study in Flemish GPs. BMJ Open 2020;10:e039674. https://doi.org/10.1136/bmjope....
12.
WHO b. Community-based health care, including outreach and campaigns, in the context of the COVID-19 pandemic. Interim guidance. May 2020. Switzerland: Geneva. https://apps.who.int/iris/hand... (access 2022.8.28).
13.
The Health Policy Partnership. Out of the ashes: why prioritising non-communicable diseases is central to post-COVID-19 recovery. London. The Health Policy Partnership. 2021, 21 p.
14.
Castelltort PP, Oliver RLS, Opulencia JBA, et al. Teleconsultation for Medical Doctors. Int J Cybern Inform. 2022;11(4):135–155. https://doi.org/10.5121/ijci.2....
15.
Devi R, Goodyear-Smith F, Subramaniam K, et al. The Impact of COVID-19 on the Care of Patients With Noncommunicable Diseases in Low- and Middle-Income Countries: An Online Survey of Patient Perspectives. J Patient Exp. 2021;8:23743735211034091. https://doi.org/10.1177/237437....
16.
Těšinová JK, Dobiášová K. Využívání informačně komunikačních technologií v primární péči v době pandemie covidu-19 perspektivou pacientů. Medicína po promoci. 2022;2022(2).
17.
Monaco A, Palmer K, Holm Ravn Faber N, et al. Digital Health Tools for Managing Noncommunicable Diseases During and After the COVID-19 Pandemic: Perspectives of Patients and Caregivers. J Med Internet Res. 2021;23(1):e25652. https://doi.org/10.2196/25652.
18.
Russell A, De Wildt G, Grut M, et al. What can general practice learn from primary care nurses’ and healthcare assistants‘experiences of the COVID-19 pandemic? BMJ Open. 2022;12(3):e055955. https://doi.org/10.1136/bmjope....
19.
Carpenter JS, Draucker CB, Bartlett Ellis R, et al. Indiana University Health Nursing COVID-19 Spirit of Inquiry and Innovation. Descriptive Qualitative Study. Nurs Outlook. 2022;70(1):137–144. https://doi.org/10.1016/j.outl....
20.
Alwani SS, Majeed MM, Ramzan Z, et al. Evaluation of knowledge, practices, attitude, and anxiety of nurses towards COVID-19 during the current outbreak in Karachi, Pakistan. Pak J Public Health. 2021;10(2):82–90.
21.
Arnetz JE, Goetz CM, Arnetz BB, et al. Nurse Reports of Stressful Situations during the COVID-19 Pandemic: Qualitative Analysis of Survey Responses. Int J Environ Res Public Health. 2020;17(21):8126. https://doi.org/10.3390/ijerph....
22.
Cui S, Jiang Y, Shi Q, et al. Impact of COVID-19 on Anxiety, Stress, and Coping Styles in Nurses in Emergency Departments and Fever Clinics: A Cross-Sectional Survey. Risk Manag Healthc Policy. 2021;14:585–594. https://doi.org/10.2147/RMHP.S....
23.
Mitchell S, Oliver P, Gardiner C, et al. Community end-of-life care during the COVID-19 pandemic: findings of a UK primary care survey. BJGP Open. 2021;5(4):BJGPO.2021.0095. https://doi.org/10.3399/BJGPO.....
24.
Zhang Y, Wei L, Li H, et al. The Psychological Change Process of Frontline Nurses Caring for Patients with COVID-19 during Its Outbreak. Issues Ment Health Nurs. 2020;41(6):525–530. https://doi.org/10.1080/016128....
25.
Sarwar MAA, Sarwar H. The Impact of COVID-19 on the Mental Health of Healthcare Professionals. J Coll Physicians Surg Pak. 2020;30(6):83. https://doi.org/10.29271/jcpsp....
26.
Halata D, Javorská K, Býma S, et al. Názory občanů České republiky na vybrané aspekty činnosti všeobecných praktických lékařů – 2020. Prakt Lek. 2021;101(5):261–267.
27.
Chen SC, Lai YH, Tsay SL. Nursing Perspectives on the Impacts of COVID-19. J Nurs Res. 2020;28(3):1–4. https://doi.org/10.1097/jnr.00....
28.
Gordon CH, Thompson A. Use of personal protective equipment during the COVID-19 pandemic. Br J Nurs. 2020;29(13):748–752. https://doi.org/10.12968/bjon.....
29.
Morgantini LA, Naha U, Wang H, et al. Factors contributing to healthcare professional burnout during the COVID-19 pandemic: A rapid turnaround global survey. PLoS One. 2020;15(9):e0238217. https://doi.org/10.1371/journa....
30.
Nelson H, Hubbard Murdoch N, Norman K. The Role of Uncertainty in the Experiences of Nurses During the Covid-19 Pandemic: A Phenomenological Study. Can J Nurs Res. 2021;53(2):124–133. https://doi.org/10.1177/084456....
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.