Online first
Current issue
Archive
Special Issues
About the Journal
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Board
Editorial Office
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
RESEARCH PAPER
Multidrug resistance of Escherichia coli isolated from the urinary bladder of dogs and cats with suspected urinary tract infections
1
ANIMALLAB Veterinary Laboratory, Warsaw, Poland
2
Institute of Psychology, Polish Academy of Sciences, Warsaw, Poland
3
Department of Sera and Vaccines Evaluation, National Institute of Public Health NIH – National Research Institute, Warsaw, Poland
Corresponding author
Ann Agric Environ Med. 2024;31(2):178-184
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
Escherichia coli is one of the most common bacteria isolated from urine samples collected from dogs and cats with urinary tract infection (UTI). Uncomplicated UTIs in dogs and cats can be treated with short courses of first-line antimicrobial drugs, e.g. amoxicillin, amoxicillin with clavulanic acid, or trimethoprim/sulfonamide. Recurrent or complicated UTIs often require long-term treatment with broad-spectrum antibiotics. However, the choice of drug should be based on antimicrobial susceptibility.
Material and methods:
Between March – September 2022, E. coli isolates cultured from the urine of 66 dogs and 41 cats with UTI symptoms were tested for antimicrobial resistance by using Minimum Inhibitory Concentration (MIC). Antimicrobial susceptibility was tested for ampicillin, ampicillin/sulbactam, cefazolin, cefuroxime, aztreonam, gentamycin, amikacin, colistin, trimethoprim/sulfamethoxazole, ciprofloxacin, chloramphenicol and tetracycline.
Results:
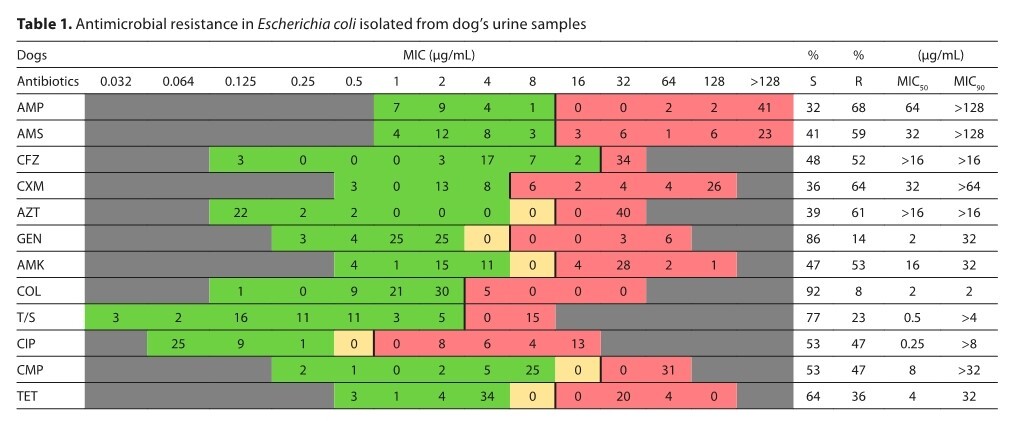
The highest prevalence of resistance was documented for ampicillin (68% in dogs, 100% in cats) and ampicillin with sulbactam (59% in dogs, 54% in cats). The most common antimicrobial resistance patterns of E. coli were ampicillin alone (12 isolates, 29.3% in cats) and beta-lactams, including aztreonam (14 isolates, 21.2% in dogs).
Conclusions:
High resistance to aztreonam (61% and 32% of isolates from dogs and cats, respectively), other beta-lactams, and fluoroquinolones should cause be alarm due to zoonotic potential and cross-transmission of antimicrobial-resistant microorganisms between animals and humans.
Escherichia coli is one of the most common bacteria isolated from urine samples collected from dogs and cats with urinary tract infection (UTI). Uncomplicated UTIs in dogs and cats can be treated with short courses of first-line antimicrobial drugs, e.g. amoxicillin, amoxicillin with clavulanic acid, or trimethoprim/sulfonamide. Recurrent or complicated UTIs often require long-term treatment with broad-spectrum antibiotics. However, the choice of drug should be based on antimicrobial susceptibility.
Material and methods:
Between March – September 2022, E. coli isolates cultured from the urine of 66 dogs and 41 cats with UTI symptoms were tested for antimicrobial resistance by using Minimum Inhibitory Concentration (MIC). Antimicrobial susceptibility was tested for ampicillin, ampicillin/sulbactam, cefazolin, cefuroxime, aztreonam, gentamycin, amikacin, colistin, trimethoprim/sulfamethoxazole, ciprofloxacin, chloramphenicol and tetracycline.
Results:
The highest prevalence of resistance was documented for ampicillin (68% in dogs, 100% in cats) and ampicillin with sulbactam (59% in dogs, 54% in cats). The most common antimicrobial resistance patterns of E. coli were ampicillin alone (12 isolates, 29.3% in cats) and beta-lactams, including aztreonam (14 isolates, 21.2% in dogs).
Conclusions:
High resistance to aztreonam (61% and 32% of isolates from dogs and cats, respectively), other beta-lactams, and fluoroquinolones should cause be alarm due to zoonotic potential and cross-transmission of antimicrobial-resistant microorganisms between animals and humans.
REFERENCES (49)
1.
Dorsch R, Teichmann-Knorrn S, Sjetne Lund H. Urinary tract infection and subclinical bacteriuria in cats: A clinical update. J Feline Med Surg. 2019;21(11):1023–1038. https://doi.org/10.1177/109861....
2.
Weese JS, Blondeau J, Boothe D, et al. International Society for Companion Animal Infectious Diseases (ISCAID) guidelines for the diagnosis and management of bacterial urinary tract infections in dogs and cats. Vet J. 2019;247:8–25. https://doi.org/10.1016/j.tvjl....
3.
Walker GK, Yustyniuk V, Shamoun J, et al. Detection of Escherichia coli and Enterococcus spp. in dogs with polymicrobial urinary tract infections: A 5-year retrospective study. J Vet Intern Med. 2022;36(4):1322–1329. https://doi.org/10.1111/jvim.1....
4.
Wong C, Epstein SE, Westropp JL. Antimicrobial Susceptibility Patterns in Urinary Tract Infections in Dogs (2010–2013). J Vet Intern Med. 2015;29(4):1045–52. https://doi.org/10.1111/jvim.1....
5.
Thompson MF, Litster AL, Platell JL, et al. Canine bacterial urinary tract infections: new developments in old pathogens. Vet J. 2011;190(1):22–7. https://doi.org/10.1016/j.tvjl....
6.
Garces A, Lopes R, Silva A, et al. Bacterial Isolates from Urinary Tract Infection in Dogs and Cats in Portugal, and Their Antibiotic Susceptibility Pattern: A Retrospective Study of 5 Years (2017–2021). Antibiotics (Basel). 2022;11(11):1520. https://doi.org/10.3390/antibi....
7.
Amphaiphan C, Yano T, Som-in M, et al. Antimicrobial drug resistance profile of isolated bacteria in dogs and cats with urologic problems at Chiang Mai University Veterinary Teaching Hospital, Thailand (2012–2016). Zoonoses Public Health. 2021;68:452–63. https://doi.org/10.1111/zph.12....
8.
Yudhanto S, Hung CC, Maddox CW, et al. Antimicrobial Resistance in Bacteria Isolated From Canine Urine Samples Submitted to a Veterinary Diagnostic Laboratory, Illinois, United States. Front Vet Sci. 2022;9:867784. https://doi.org/10.3389/fvets.....
9.
European Centre for Disease Prevention and Control. Factsheet for experts – Antimicrobial resistance. https://www.ecdc.europa.eu/en/... (acces: 23.10.2023).
10.
Hernando E, Vila A, D’Ippolito P, et al. Prevalence and Characterization of Urinary Tract Infection in Owned Dogs and Cats From Spain. Top. Companion Anim. Med. 2021;43:100512. https://doi.org/10.1016/j.tcam....
11.
Bartges JW. Diagnosis of urinary tract infections. Vet Clin N Am Small Anim Pract. 2004;34:923–33. https://doi.org/10.1016/j.cvsm....
12.
Marques C, Gama LT, Belas A, et al. European multicenter study on antimicrobial resistance in bacteria isolated from companion animal urinary tract infections. BMC Vet Res. 2016;12:213. https://doi.org/10.1186/s12917....
13.
Teichmann-Knorrn S, Reese S, Wolf G, et al. Prevalence of feline urinary tract pathogens and antimicrobial resistance over five years. Vet Rec. 2018;183(1):21. https://doi.org/10.1136/vr.104....
14.
Yu Z, Wang Y, Chen Y, et al. Antimicrobial resistance of bacterial pathogens isolated from canine urinary tract infections. Vet Microbiol. 2020;241:108540. https://doi.org/10.1016/j.vetm....
15.
Smoglica C, Evangelisti G, Fani C, et al. Antimicrobial Resistance Profile of Bacterial Isolates from Urinary Tract Infections in Companion Animals in Central Italy. Antibiotics (Basel). 2022;11(10):1363. https://doi.org/10.3390/antibi....
16.
CLSI. Performance Standards for Antimicrobial Disk and Dilution Susceptibility Tests for Bacteria Isolated from Animals, 4th Edition. CLSI Supplement VET08. Wayne, PA: Clinical and Laboratory Standards Institute; 2018.
17.
CLSI. Performance standards for antimicrobial disk and dilution susceptibility tests for bacteria isolated from animals. CLSI Report VET01S ED5:2020.
18.
CLSI. Performance Standards for Antimicrobial Susceptibility Testing. 29th Edition. CLSI Supplement M100. Wayne, PA: Clinical and Laboratory Standards Institute; 2019.
19.
Rodríguez-Gascón A, Aguirre-Quinonero A, Canut-Blasco A. Are oral cefuroxime axetil, cefixime and cefditoren pivoxil adequate to treat uncomplicated acute pyelonephritis after switching from intravenous therapy? A pharmacokinetic/pharmacodynamic perspective. Enferm Infecc Microbiol Clin (Engl Ed). 2020;38(7):306–311. https://doi.org/10.1016/j.eimc....
20.
Feßler AT, Scholtzek AD, Schug AR, et al. Antimicrobial and Biocide Resistance among Canine and Feline Enterococcus faecalis, Enterococcus faecium, Escherichia coli, Pseudomonas aeruginosa, and Acinetobacter baumannii Isolates from Diagnostic Submissions. Antibiotics (Basel). 2022;11(2):152. https://doi.org/10.3390/antibi....
21.
Authority EFS. The European Union Summary Report on Antimicrobial Resistance in zoonotic and indicator bacteria from humans, animals and food in 2018/2019. EFSA J. 2021;19:e06490. https://doi.org/10.2903/j.efsa....
22.
Stefaniuk E, Suchocka U, Bosacka K, et al. Etiology and antibiotic susceptibility of bacterial pathogens responsible for community-acquired urinary tract infections in Poland. Eur J Clin Microbiol Infect Dis. 2016;35:1363–1369. https://doi.org/10.1007/s10096....
23.
van Driel AA, Notermans DW, Meima A, et al. Antibiotic resistance of Escherichia coli isolated from uncomplicated UTI in general practice patients over a 10-year period. Eur J Clin Microbiol Infect Dis. 2019;38(11):2151–2158. https://doi.org/10.1007/s10096....
24.
Rampacci E, Bottinelli M, Stefanetti V, et al. Antimicrobial susceptibility survey on bacterial agents of canine and feline urinary tract infections: Weight of the empirical treatment. J Glob Antimicrob Resist. 2018;13:192–196. https://doi.org/10.1016/j.jgar....
25.
Moyaert H, Morrissey I, de Jong A, et al. Antimicrobial Susceptibility Monitoring of Bacterial Pathogens Isolated from Urinary Tract Infections in Dogs and Cats Across Europe: ComPath Results. Microb Drug Resist. 2017;23(3):391–403. https://doi.org/10.1089/mdr.20....
26.
Rzewuska M, Czopowicz M, Kizerwetter-Świda M, et al. Multidrug resistance in Escherichia coli strains isolated from infections in dogs and cats in Poland (2007–2013) The Scientific World Journal. 2015;2015:408205. https://doi.org/10.1155/2015/4....
27.
Johnstone T. A clinical approach to multidrug-resistant urinary tract infection and subclinical bacteriuria in dogs and cats. NZVet J. 2020;68(2):69–83. https://doi.org/10.1080/004801....
28.
Fonseca JD, Mavrides DE, Graham PA, et al. Results of Urinary Bacterial Cultures and Antibiotic Susceptibility Testing of Dogs and Cats in the UK. J Small Anim Pract. 2021;62:1085–1091. https://doi.org/10.1111/jsap.1....
29.
Warzecha D, Pietrzak B, Urban A, et al. How to avoid drug resistance during treatment and prevention of urinary tract infections. Prz Menopauzalny. 2021;20(4):217–221. https://doi.org/10.5114/pm.202....
30.
Davis WH, Magee MR, Monks SM, et al. Assessment of nationally recommended antibiotics for treatment of UTI in U.S.-Mexico border emergency departments. Am J Emerg Med. 2022;61:12–17. https://doi.org/10.1016/j.ajem....
31.
Haddad JM, Ubertazzi E, Cabrera OS, et al. Latin American consensus on uncomplicated recurrent urinary tract infection-2018. Int Urogynecol J. 2020;31(1):35–44. https://doi.org/10.1007/s00192....
32.
Jurałowicz E, Bartoszko-Tyczkowska A, Tyczkowska-Sieroń E, et al. Etiology and bacterial susceptibility to antibiotics in patients with recurrent lower urinary tract infections. Pol Arch Intern Med. 2020;130:373–381. https://doi.org/10.20452/pamw.....
33.
Stompór T. Recurrent lower urinary tract infections in adults: don’t think it’s E. coli, don’t choose ciprofloxacin to treat. Pol Arch Intern Med. 2020;130:368–370. https://doi.org/10.20452/pamw.....
34.
Daniels JB, Tracy G, Irom SJ, et al. Fluoroquinolone levels in healthy dog urine following a 20-mg/kg oral dose of enrofloxacin exceed mutant prevention concentration targets against Escherichia coli isolated from canine urinary tract infections. J Vet Pharmacol Ther. 2014;37(2):201–4. https://doi.org/10.1111/jvp.12....
35.
Papich MG. Ciprofloxacin Pharmacokinetics in Clinical Canine Patients. J Vet Intern Med. 2017;31(5):1508–1513. https://doi.org/10.1111/jvim.1....
36.
Byrne MK, Miellet S, McGlinn A, et al. The drivers of antibiotic use and misuse: the development and investigation of a theory driven community measure. BMC Public Health. 2019;19(1):1425. https://doi.org/10.1186/s12889....
37.
Martins IJ, Brito ACF, Santos AL, et al. Multidrug-resistant Escherichia coli isolated from a dog with a history of urolithiasis: case report. Arq bras med vet zootec. 2020;72(3):931–935. https://doi.org/10.1590/1678-4....
38.
Growcott EJ, Cariaga TA, Morris L, et al. Pharmacokinetics and pharmacodynamics of the novel monobactam LYS228 in a neutropenic murine thigh model of infection. J Antimicrob Chemother. 2019;74(1):108–116. https://doi.org/10.1093/jac/dk....
39.
Noel AR, Attwood M, Bowker KE, et al. Pharmacodynamics of aztreonam against Escherichia coli and Klebsiella oxytoca: defining pharmacodynamic targets. J Antimicrob Chemother. 2020;75(3):772–773. https://doi.org/10.1093/jac/dk....
40.
Nordmann P, Yao Y, Falgenhauer L, et al. Recent Emergence of Aztreonam-Avibactam Resistance in NDM and OXA-48 Carbapenemase-Producing Escherichia coli in Germany. Antimicrob Agents Chemother. 2021;65(11):e0109021. https://doi.org/10.1128/AAC.01....
41.
Marchetti L, Buldain D, Gortari Castillo L, et al. Pet and Stray Dogs as Reservoirs of Antimicrobial-Resistant Escherichia coli. Int J Microbiol. 2021;2021:6664557. https://doi.org/10.1155/2021/6....
42.
Bahadori M, Motamedifar M, Derakhshandeh A, et al. Genetic relatedness of the Escherichia coli fecal population and strains causing urinary tract infection in the same host. Microbiologyopen. 20198(6):e00759. https://doi.org/10.1002/mbo3.7....
43.
Scott A, Pottenger S, Timofte D, et al. Reservoirs of resistance: polymyxin resistance in veterinary-associated companion animal isolates of Pseudomonas aeruginosa. Vet Rec. 2019;185(7):206. https://doi.org/10.1136/vr.105....
44.
Sharma J, Sharma D, Singh A, et al. Colistin Resistance and Management of Drug Resistant Infections. Can J Infect Dis Med Microbiol. 2022;2022:4315030. https://doi.org/10.1155/2022/4....
45.
Oishi N, Talaska AE, Schacht J. Ototoxicity in dogs and cats. Vet Clin North Am Small Anim Pract. 2012;42(6):1259–71. https://doi.org/10.1016/j.cvsm....
46.
Gaire TN, Scott HM, Sellers L, et al. Age Dependence of Antimicrobial Resistance Among Fecal Bacteria in Animals: A Scoping Review. Front Vet Sci. 2021;7:622495. https://doi.org/10.3389/fvets.....
47.
Hossain A, Hossain SA, Fatema AN, et al. Age and gender-specific antibiotic resistance patterns among Bangladeshi patients with urinary tract infection caused by Escherichia coli. Heliyon. 2020;6(6):e04161. https://doi.org/10.1016/j.heli....
48.
Naziri Z, Poormaleknia M, Ghaedi Oliyaei A. Risk of sharing resistant bacteria and/or resistance elements between dogs and their owners. BMC Vet Res. 2022;18(1):203. https://doi.org/10.1186/s12917....
49.
Damborg P, Pirolo M, Schon Poulsen L, et al. Dogs Can Be Reservoirs of Escherichia coli Strains Causing Urinary Tract Infection in Human Household Contacts. Antibiotics (Basel). 2023;12(8):1269. https://doi.org/10.3390/antibi....
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.