Online first
Current issue
Archive
Special Issues
About the Journal
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Board
Editorial Office
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
RESEARCH PAPER
Characteristics of osteoporotic vertebral fractures in association with symptomatic status in postmenopausal women – a retrospective study of a single centre in Poland
1
Department of Rheumatology, Systemic Connective Tissue Diseases and Rare Diseases, Central Clinical Hospital MSWiA, Warsaw, Poland
2
Department of Geriatrics, Internal Medicine and Metabolic Bone Diseases, Centre of Postgraduate Medical Education,
Warsaw, Poland
3
Department of Family Medicine, Medical University, Warsaw, Poland
4
School of Public Health, Centre of Postgraduate Medical Education, Warsaw, Poland
5
Department of Social Medicine, Medical University, Łódź, Poland
6
University of Humanities and Economics, Łódź, Poland
Ann Agric Environ Med. 2021;28(4):654-658
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
Vertebral compression fractures (VCFs), which are a complication of osteoporosis, often cause diagnostic and therapeutic difficulties. The aim of this study was to find association between the characteristics of VCFs and the symptomatic status of patients.
Material and methods:
The study involved a total of 437 women with diagnosed postmenopausal osteoporosis (193 with at least one compression fracture and 244 without VCFs). To identify VCFs, all patients underwent morphometry using dual-energy X-ray absorptiometry. Based on the history of VCFs, subjects were divided into two groups: with symptomatic (n=59) and asymptomatic (n=134) VCFs.
Results:
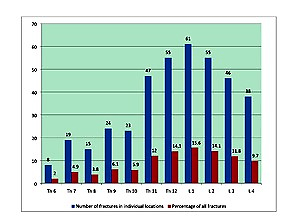
Each patient had, on average, 2.03 ± 1.50 VCFs. Patients with VCFs were older [p<0.001] and shorter [p<0.001] than those without VCFs. VCFs located in the thoracic spine and the lumbar spine occurred with similar frequency (p=0.112). Multiple fractures in both spine segments (50.13%) were more frequent than fractures limited to only one section of the spine, either thoracic (22.76%) or lumbar (27.11%). The decreasing number of subjects was exponentially associated with the increasing number of VCFs (p<0.001). Symptomatic patients compared to asymptomatic patients had a higher serum concentration of 25-hydroxyvitamin D, and lower serum activity of alkaline phosphatase (p<0.01; p<0.005, respectively). In the lumbar spin, the risk of symptomatic VCFs was more than twofold higher compared to asymptomatic VCFs (p <0.001, OR=2.57, 95% CI: 1.57–4.19). Symptomatic status depended on the number of lumbar VCFs (p<0.001, OR=2.47, 95% CI: 1.68–3.63), as well as higher T-score L1-L4 (p=0.009, OR=1.43, 95% CI: 1.09–1.88).
Conclusions:
Patients’ symptomatic status depends on the location and number of VCFs, as well as T-score L1-L4.
Vertebral compression fractures (VCFs), which are a complication of osteoporosis, often cause diagnostic and therapeutic difficulties. The aim of this study was to find association between the characteristics of VCFs and the symptomatic status of patients.
Material and methods:
The study involved a total of 437 women with diagnosed postmenopausal osteoporosis (193 with at least one compression fracture and 244 without VCFs). To identify VCFs, all patients underwent morphometry using dual-energy X-ray absorptiometry. Based on the history of VCFs, subjects were divided into two groups: with symptomatic (n=59) and asymptomatic (n=134) VCFs.
Results:
Each patient had, on average, 2.03 ± 1.50 VCFs. Patients with VCFs were older [p<0.001] and shorter [p<0.001] than those without VCFs. VCFs located in the thoracic spine and the lumbar spine occurred with similar frequency (p=0.112). Multiple fractures in both spine segments (50.13%) were more frequent than fractures limited to only one section of the spine, either thoracic (22.76%) or lumbar (27.11%). The decreasing number of subjects was exponentially associated with the increasing number of VCFs (p<0.001). Symptomatic patients compared to asymptomatic patients had a higher serum concentration of 25-hydroxyvitamin D, and lower serum activity of alkaline phosphatase (p<0.01; p<0.005, respectively). In the lumbar spin, the risk of symptomatic VCFs was more than twofold higher compared to asymptomatic VCFs (p <0.001, OR=2.57, 95% CI: 1.57–4.19). Symptomatic status depended on the number of lumbar VCFs (p<0.001, OR=2.47, 95% CI: 1.68–3.63), as well as higher T-score L1-L4 (p=0.009, OR=1.43, 95% CI: 1.09–1.88).
Conclusions:
Patients’ symptomatic status depends on the location and number of VCFs, as well as T-score L1-L4.
ACKNOWLEDGEMENTS
Ethical aspects. Research protocols were approved by
the Ethics Committee of the Centre for Postgraduate
Medical Education in Warsaw (No. 64/PB/2018). The study
complied with the 1964 Declaration of Helsinki with its later
amendments. All participants received detailed instructions
regarding the protocols and written consent was obtained
from all patients.
REFERENCES (34)
1.
Lorentzon M, Branco J, Brandi ML, et al. Algorithm for the Use of Biochemical Markers of Bone Turnover in the Diagnosis, Assessment and Follow-Up of Treatment for Osteoporosis. Adv Ther. 2019; 36(10): 2811–2824. https://doi.org/10.1007/s12325....
2.
Janiszewska M, Kulik T, Dziedzic M, et al. Knowledge of osteoporosis prophylaxis and health behaviours of the population of chosen countries of the world. Ann Agric Environ Med. 2014; 21(2): 364–368. https://doi.org/10.5604/1232-1....
3.
Schousboe J, Vo T, Taylor B. Prediction of Incident Major Osteoporotic and Hip Fractures by Trabecular Bone Score (TBS) and Prevalent Radiographic Vertebral Fracture in Older Men. J Bone Miner Res. 2016; 31(3): 690–697. https://doi.org:10.1002/jbmr.2....
4.
Rud B, Vestergaard A, Hyldstrup L. Accuracy of densitometric vertebral fracture assessment when performed by DXA technicians--a cross-sectional, multiobserver study. Osteoporos Int. 2016; 27(4): 1451–1458. https://doi.org/10.1007/s00198....
5.
Karlsson M, Kherad M, Hasserius R, et al. Characteristics of Prevalent Vertebral Fractures Predict New Fractures in Elderly Men. J Bone Joint Surg Am. 2016; 98(5): 379–385. https://doi.org/10.2106/JBJS.1....
6.
McCarthy J, Davis A. Diagnosis and Management of Vertebral Compression Fractures. Am Fam Physician. 2016; 94(1): 44–50.
7.
Zeytinoglu M, Jain R, Vokes T. Vertebral fracture assessment: Enhancing the diagnosis, prevention, and treatment of osteoporosis. Bone. 2017; 104: 54–65. https://doi.org/10.1016/j.bone....
8.
Cicala D, Briganti F, Casale L, et al. Atraumatic vertebral compression fractures: differential diagnosis between benign osteoporotic and malignant fractures by MRI. Musculoskelet Surg. 2013; 97 Suppl 2: S169–179. https://doi.org/10.1007/s12306....
9.
Balasubramanian A, Zhang J, Chen L, et al. Risk of subsequent fracture after prior fracture among older women. Osteoporos Int. 2019; 30(1): 79–92. https://doi.org/10.1007/s00198....
10.
Wu Q, Xiao X, Xu Y. Evaluating the Performance of the WHO International Reference Standard for Osteoporosis Diagnosis in Postmenopausal Women of Varied Polygenic Score and Race. J Clin Med. 2020; 9(2): 499. https://doi.org/10.3390/jcm902....
11.
Kanis JA, Cooper C, Rizzoli R, et al. Scientific Advisory Board of the European Society for Clinical and Economic Aspects of Osteoporosis and Osteoarthritis (ESCEO) and the Committees of Scientific Advisors and National Societies of the International Osteoporosis Foundation (IOF). Executive summary of the European guidance for the diagnosis and management of osteoporosis in postmenopausal women. Calcif Tissue Int. 2019; 104(3): 235–238. https://doi.org/10.1007/s00223....
12.
Muszkat P, Camargo M, Peters B, et al. Digital vertebral morphometry performed by DXA: a valuable opportunity for identifying fractures during bone mass assessment. Arch Endocrinol Metab. 2015; 59(2): 98–104. https://doi.org/10.1590/2359-3....
13.
Wood K, Li W, Lebl D, et al. Management of thoracolumbar spine fractures. Spine J. 2014; 14(1): 145–164. https://doi.org/10.1016/j.spin....
14.
Stanghelle B, Bentzen H, Giangregorio L, et al. Associations between health-related quality of life, physical function and pain in older women with osteoporosis and vertebral fracture. BMC Geriatr. 2019; 19: 298. https://doi.org/10.1186/s12877....
15.
Che H, Breuil V, Cortet B, et al. Vertebral fractures cascade: potential causes and risk factors. Osteoporos Int. 2019; 30(3): 555–563. https://doi.org/10.1007/s00198....
16.
Van der Velde R, Ozanian T, Dumitrescu B, et al. Performance of statistical models of shape and appearance for semiautomatic segmentations of spinal vertebrae T4-L4 on digitized vertebral fracture assessment images. Spine J. 2015; 15(6): 1248–1254. https://doi.org/10.1016/j.spin....
17.
Oh S, Kim D, Lee Y, et al. Comparison of screening strategies for prevalent vertebral fractures in South Korea: vertebral fracture assessment vs. spine radiograph. BMC Musculoskelet Disord. 2018; 19(1): 46. https://doi.org/10.1186/s12891....
18.
Shetty S, John B, Mohan S, et al. Vertebral fracture assessment by dual-energy X-ray absorptiometry along with bone mineral density in the evaluation of postmenopausal osteoporosis. Arch Osteoporos. 2020; 15(1): 25. https://doi.org/10.1007/s11657....
19.
Dennison E, Cooper C, Kanis J, et al. Fracture risk following intermission of osteoporosis therapy. Osteoporos Int. 2019; 30(9): 1733–1743. https://doi.org/10.1007/s00198....
20.
Cummings S, Ferrari S, Eastell R, et al. Vertebral Fractures After Discontinuation of Denosumab: A Post Hoc Analysis of the Randomized Placebo-Controlled FREEDOM Trial and Its Extension. J Bone Miner Res. 2018; 33(2): 190–198. https://doi.org/10.1002/jbmr.3....
21.
Vandenbroucke A, Luyten F, Flamaing J, et al. Pharmacological treatment of osteoporosis in the oldest old. Clin Interv Aging. 2017; 12: 1065–1077. https://doi.org/10.2147/CIA.S1....
22.
Nurmi-Lüthje I, Lüthje P, Kaukonen J, et al. Positive Effects of a Sufficient Pre-fracture Serum Vitamin D Level on the Long-Term Survival of Hip Fracture Patients in Finland: A Minimum 11-Year Follow-Up. Drugs Aging. 2015; 32(6): 477–486. https://doi.org/10.1007/s40266....
23.
Bone HG, Wagman RB, Brandi ML, et al. 10 years of denosumab treatment in postmenopausal women with osteoporosis: results from the phase 3 randomised FREEDOM trial and open-label extension. Lancet Diabetes Endocrinol. 2017; 5(7): 513–523. https://doi.org/10.1016/S2213-....
24.
Janiszewska M, Firlej E, Dziedzic M, et al. Health beliefs and sense of one’s own efficacy and prophylaxis of osteoporosis in peri- and post-menopausal women. Ann Agric Environ Med. 2016; 23(1): 167–173. https://doi.org/10.5604/123219....
25.
Al-Sari U, Tobias J, Clark E. Health-related quality of life in older people with osteoporotic vertebral fractures: a systematic review and meta-analysis. Osteoporos Int. 2016; 27(10): 2891–2900. https://doi.org/10.1007/s00198....
26.
Aebi M, Maas C, Di Pauli von Treuheim T, et al. Comparative biomechanical study of a new transpedicular vertebral device and vertebroplasty for the treatment or prevention of vertebral compression fractures. Clin Biomech (Bristol, Avon). 2018; 56: 40–45. https://doi.org/10.1016/j.clin....
27.
Kanis JA, Johansson H, Odén A, et al. Characteristics of recurrent fractures. Osteoporos Int. 2018; 29(8): 1747–1757. doi: 10.1007/s00198-018-4502-0.
28.
Johansson H, Odén A, McCloskey E, et al. Mild morphometric vertebral fractures predict vertebral fractures but not non-vertebral fractures. Osteoporos Int. 2014; 25(1): 235–241. https://doi.org/10.1007/s00198....
29.
Ren H, Jiang J, Chen J, et al. Risk factors of new symptomatic vertebral compression fractures in osteoporotic patients undergone percutaneous vertebroplasty. Eur Spine J. 2015; 24(4): 750–758. https://doi.org/10.1007/s00586....
30.
Simpson EL, Martyn-St James M, Hamilton J, et al. Clinical effectiveness of denosumab, raloxifene, romosozumab, and teriparatide for the prevention of osteoporotic fragility fractures: A systematic review and network meta-analysis. Bone. 2020; 130: 115081. https:// doi.org/10.1016/j.bone.2019.115081.
31.
Iconaru L, Moreau M, Kinnard V, et al. Does the Prediction Accuracy of Osteoporotic Fractures by BMD and Clinical Risk Factors Vary With Fracture Site? JBMR Plus. 2019; 3(12): e10238. https://doi.org/10.1002/jbm4.1....
32.
Okubo N, Matsui S, Matsumoto T, et al. Relationship Between Bone Mineral Density and Risk of Vertebral Fractures with Denosumab Treatment in Japanese Postmenopausal Women and Men with Osteoporosis. Calcif Tissue Int. 2020; 107(6): 559–566. https://doi.org/10.1007/s00223....
33.
Bouxsein ML, Eastell R, Lui LY, et al. Change in Bone Density and Reduction in Fracture Risk: A Meta-Regression of Published Trials. J Bone Miner Res. 2019; 34(4): 632–642. https://doi.org/10.1002/jbmr.3....
34.
Drampalos E, Nikolopoulos K, Baltas C, et al. Vertebral fracture assessment: Current research status and application in patients with kyphoplasty. World J Orthop. 2015 Oct 18; 6(9): 680–687. https://doi.org/10.5312/wjo.v6....
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.