Online first
Current issue
Archive
Special Issues
About the Journal
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Board
Editorial Office
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
CASE REPORT
Osteomyelitis caused by co-infection of Citrobacter freundii and Morganella morganii following soil exposure – Case Report and Clinical Insights
1
Department of Dermatology, 4th Affiliated Hospital of Southwest Medical University (TIANFU Affiliated Hospital), China
2
Orthopaedics Department, Renshou County Traditional Chinese Medicine Hospital, China
3
Department of Neurology, 4th Affiliated Hospital of Southwest Medical University, China
Corresponding author
Yang Xu
Department of dermatology, The Fourth Affiliated Hospital of Southwest Medical University (TIANFU Affiliated Hospital), China
Department of dermatology, The Fourth Affiliated Hospital of Southwest Medical University (TIANFU Affiliated Hospital), China
KEYWORDS
TOPICS
ABSTRACT
Introduction:
Soil harbours diverse bacteria and antibiotic resistance genes. This report describes a rare co-infection with Citrobacter freundii (C. freundii) and Morganella morganii (M. morganii) causing hand osteomyelitis in an elderly farmer, highlighting dynamic pathogen shifts and management challenges.
Case Report:
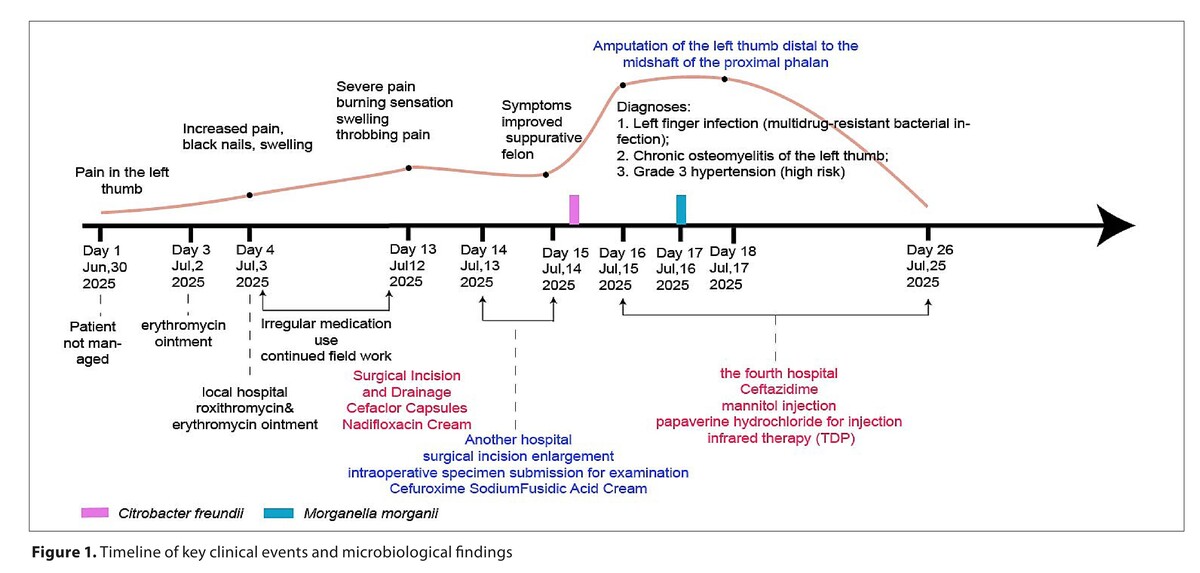
An 85-year-old farmer developed a thumb felon after fieldwork. Treatment failure and non-compliance led to progression. Despite repeated drainage and antibiotics, osteomyelitis developed. Sequential cultures showed a shift from C. freundii to M. morganii. Distal thumb amputation was ultimately required, resulting in permanent disability.
Results and Conclusions:
Soil exposure can cause sequential polymicrobial infections. Inadequate treatment disrupts local ecology, favouring resistant bacteria. Dynamic microbiological monitoring is essential. A strategy of ‘continuous monitoring + ecological antimicrobial selection + proactive MDT involvement’ is recommended for high-risk individuals.
Soil harbours diverse bacteria and antibiotic resistance genes. This report describes a rare co-infection with Citrobacter freundii (C. freundii) and Morganella morganii (M. morganii) causing hand osteomyelitis in an elderly farmer, highlighting dynamic pathogen shifts and management challenges.
Case Report:
An 85-year-old farmer developed a thumb felon after fieldwork. Treatment failure and non-compliance led to progression. Despite repeated drainage and antibiotics, osteomyelitis developed. Sequential cultures showed a shift from C. freundii to M. morganii. Distal thumb amputation was ultimately required, resulting in permanent disability.
Results and Conclusions:
Soil exposure can cause sequential polymicrobial infections. Inadequate treatment disrupts local ecology, favouring resistant bacteria. Dynamic microbiological monitoring is essential. A strategy of ‘continuous monitoring + ecological antimicrobial selection + proactive MDT involvement’ is recommended for high-risk individuals.
REFERENCES (23)
1.
Roesch LF, Fulthorpe RR, Riva A, et al. Pyrosequencing enumerates and contrasts soil microbial diversity. ISME J. 2007;1(4):283–90. doi:10.1038/ismej.2007.53.
2.
Nesme J, Cécillon S, Delmont TO, et al. Large-scale metagenomic-based study of antibiotic resistance in the environment. Curr Biol. 2014;24(10):1096–100. doi:10.1016/j.cub.2014.03.036.
3.
Anedda E, Ekhlas D, Alexa E, et al. Characterization of antimicrobial resistant Enterobacterales isolated from spinach and soil following zinc amendment. Environ Pollut. 2024;361:124774. doi:10.1016/j.envpol.2024.124774.
4.
Liu H, Zhu J, Hu Q, Rao X. Morganella morganii, a non-negligent opportunistic pathogen. Int J Infect Dis. 2016;50:10–7. doi:10.1016/j.ijid.2016.07.006.
5.
Flevas DA, Syngouna S, Fandridis E, et al. Infections of the hand: an overview. EFORT Open Rev. 2019;4(5):183–93. doi:10.1302/2058-5241.4.180082.
6.
Stricker T, Fröhlich S, Nadal D. Osteomyelitis and septic arthritis due to Citrobacter freundii and Haemophilus influenzae type b. J Paediatr Child Health. 1998;34(1):90–1. doi:10.1046/j.1440-1754.1998.00161.x.
7.
Adhikari S, Kc S, Dev S, et al. Citrobacter freundii-associated osteomyelitis and thromboembolic events following Moderna COVID-19 vaccination: a rare case report from Nepal. Ann Med Surg (Lond). 2023;85(11):5789–94. doi:10.1097/MS9.0000000000001351.
8.
De A, Raj HJ, Maiti PK. Biofilm in osteomyelitis caused by a rare pathogen, Morganella morganii: a case report. J Clin Diagn Res. 2016;10(6):DD06–8. doi:10.7860/JCDR/2016/18666.7990.
9.
Lee H, Hong Y, Kim M. Structural and functional changes and possible molecular mechanisms in aged skin. Int J Mol Sci. 2021;22(22):12489. doi:10.3390/ijms222212489.
10.
Suaya JA, Eisenberg DF, Fang C, Miller LG. Skin and soft tissue infections and associated complications among commercially insured patients aged 0–64 years with and without diabetes in the U.S. PLoS One. 2013;8(4):e60057. doi:10.1371/journal.pone.0060057.
11.
Ministry of Justice of the People’s Republic of China. Classification of human injury and disability [Internet]. Beijing: The Ministry; 2021 Apr 30 [updated 2021 Apr 30; cited 2025 Sep 10]. Available from: http://www.moj.gov.cn/pub/sfbg....
12.
Pulido-Cejudo A, Guzmán-Gutierrez M, Jalife-Montaño A, et al. Management of acute bacterial skin and skin structure infections with a focus on patients at high risk of treatment failure. Ther Adv Infect Dis. 2017;4(5):143–61. doi:10.1177/2049936117723228.
13.
Uberoi A, McCready-Vangi A, Grice EA. The wound microbiota: microbial mechanisms of impaired wound healing and infection. Nat Rev Microbiol. 2024;22(8):507–21. doi:10.1038/s41579-024-01035-z.
14.
Gavish N. Revisiting the exclusion principle in epidemiology at the limit of a large competitive advantage. J Theor Biol. 2025;600:112045. doi:10.1016/j.jtbi.2025.112045.
15.
Letten AD, Hall AR, Levine JM. Using ecological coexistence theory to understand antibiotic resistance and microbial competition. Nat Ecol Evol. 2021;5(4):431–41. doi:10.1038/s41559-020-01385-w16. Poirel L, Guibert M, Girlich D, et al. Cloning, sequence analyses, expression, and distribution of ampC-ampR from Morganella morganii clinical isolates. Antimicrob Agents Chemother. 1999;43(4):769–76. doi:10.1128/AAC.43.4.769.
16.
Giorgi F, Curran JM, Patterson EA. Real-time monitoring of the dynamics and interactions of bacteria and the early-stage formation of biofilms. Sci Rep. 2022;12(1):18146. doi:10.1038/s41598-022-22669-0.
17.
Young GM, Amid D, Miller VL. A bifunctional urease enhances survival of pathogenic Yersinia enterocolitica and Morganella morganii at low pH. J Bacteriol. 1996;178(22):6487–95. doi:10.1128/jb.178.22.6487-6495.1996.
18.
Falcone M, Tiseo G. Skin and soft tissue infections in the elderly. Curr Opin Infect Dis. 2023;36(2):102–8. doi:10.1097/QCO.0000000000000907.
19.
Gbinigie OA, Ordóñez-Mena JM, Fanshawe T, et al. Limited evidence for diagnosing bacterial skin infections in older adults in primary care: systematic review. BMC Geriatr. 2019;19:45. doi:10.1186/s12877-019-1061-y.
20.
Weeks LE, Scheker LR. Upper extremity wound management. J Ky Med Assoc. 1990;88(7):337–41.
21.
Costa FG, Horswill AR. Overcoming pH defenses on the skin to establish infections. PLoS Pathog. 2022;18(5):e1010512. doi:10.1371/journal.ppat.1010512.
22.
Price LB, Liu CM, Melendez JH, et al. Community analysis of chronic wound bacteria using 16S rRNA gene-based pyrosequencing: impact of diabetes and antibiotics on chronic wound microbiota. PLoS One. 2009;4(7):e6462. doi:10.1371/journal.pone.0006462.
23.
Tipton CD, Mathew ME, Wolcott RA, et al. Temporal dynamics of relative abundances and bacterial succession in chronic wound communities. Wound Repair Regen. 2017;25(4):673–9. doi:10.1111/wrr.12555.
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.