Online first
Current issue
Archive
Special Issues
About the Journal
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Board
Editorial Office
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
Editor's Choice
RESEARCH PAPER
Long-term mortality after retinal artery occlusion – a single centre study
1
Department of Ophthalmology, Regional Hospital, Kielce, Poland
2
Collegium Medicum, Jan Kochanowski University, Kielce, Poland
3
Department of Vitreoretinal Surgery, Medical University, Lublin, Poland
4
1st Clinic of Cardiology and Electrotherapy, Swietokrzyskie Cardiology Centre, Kielce, Poland
5
Ophthalmology Clinic Boni Fratres Lodziensis, Łódż, Poland
Corresponding author
Paweł Wałek
1st Clinic of Cardiology and Electrotherapy, Swietokrzyskie Cardiology Centre, Kielce, Poland
1st Clinic of Cardiology and Electrotherapy, Swietokrzyskie Cardiology Centre, Kielce, Poland
Ann Agric Environ Med. 2023;30(2):252-258
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
Retinal artery occlusion (RAO) is an ophthalmic and systemic emergency requiring urgent diagnosis and treatment. Data regarding mortality in this group, especially in the European population, are modest. The aim of this study is to assess all-cause mortality in post-RAO patients.
Material and methods:
This is a retrospective, single-centre study involving 198 patients following RAO diagnosed in 2004–2020. The control group included 198 patients after cataract surgery matched for gender and age, with the date of cataract surgery corresponding to the date of the RAO.
Results:
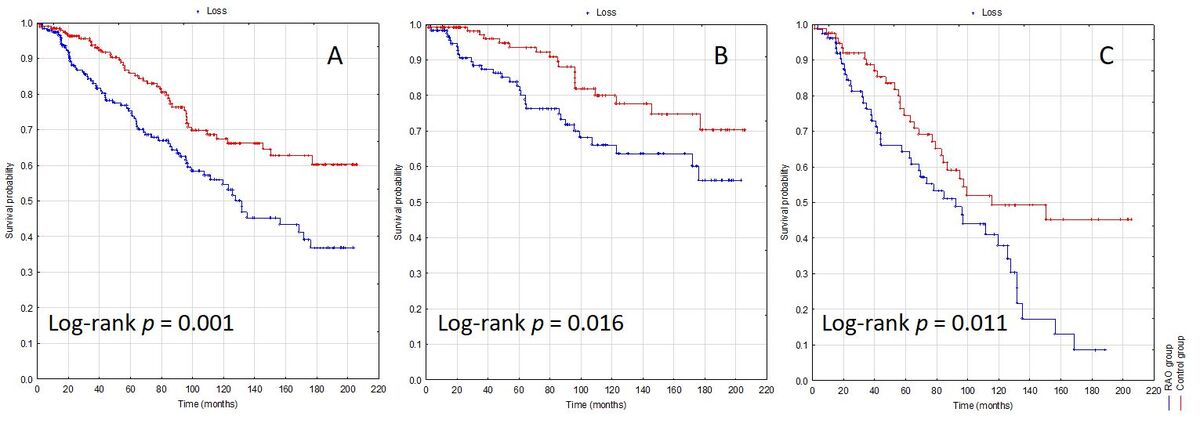
The average follow-up of the study population was 6.32±2.15 years. Post-RAO patients had significantly higher risk of all-cause mortality (Log-rank test p = 0.001), also when stratified for ages below 75 years (Log-rank test p = 0.016) and those aged 75 and over (Log-rank test p = 0.001). In the group of patients without cardiovascular events before RAO/cataract surgery, post-RAO patients were also at higher risk of all-cause mortality (Log-rank test p = 0.011), but when stratified according to age, those observations were borderline significant (Log-rank test p = 0.083 for a group of patients aged less than 75 years, and p = 0.051 for patients aged 75 and over). Cox analysis showed that in the group of post-RAO patients, the main risk factors for all-cause mortality were age (HR 1.07, 95%CI 1.04–1.1; p < 0.001), ischemic heart disease (HR 1.72; 95%CI 1.08–2.72; p = 0.022), and permanent atrial fibrillation (HR 2.18, 95%CI 1.08–4.38; p = 0.029).
Conclusions:
Regardless of age and previous cardiovascular events, post-RAO patients are at a higher risk of all-cause mortality than patients without a history of RAO.
Retinal artery occlusion (RAO) is an ophthalmic and systemic emergency requiring urgent diagnosis and treatment. Data regarding mortality in this group, especially in the European population, are modest. The aim of this study is to assess all-cause mortality in post-RAO patients.
Material and methods:
This is a retrospective, single-centre study involving 198 patients following RAO diagnosed in 2004–2020. The control group included 198 patients after cataract surgery matched for gender and age, with the date of cataract surgery corresponding to the date of the RAO.
Results:
The average follow-up of the study population was 6.32±2.15 years. Post-RAO patients had significantly higher risk of all-cause mortality (Log-rank test p = 0.001), also when stratified for ages below 75 years (Log-rank test p = 0.016) and those aged 75 and over (Log-rank test p = 0.001). In the group of patients without cardiovascular events before RAO/cataract surgery, post-RAO patients were also at higher risk of all-cause mortality (Log-rank test p = 0.011), but when stratified according to age, those observations were borderline significant (Log-rank test p = 0.083 for a group of patients aged less than 75 years, and p = 0.051 for patients aged 75 and over). Cox analysis showed that in the group of post-RAO patients, the main risk factors for all-cause mortality were age (HR 1.07, 95%CI 1.04–1.1; p < 0.001), ischemic heart disease (HR 1.72; 95%CI 1.08–2.72; p = 0.022), and permanent atrial fibrillation (HR 2.18, 95%CI 1.08–4.38; p = 0.029).
Conclusions:
Regardless of age and previous cardiovascular events, post-RAO patients are at a higher risk of all-cause mortality than patients without a history of RAO.
ACKNOWLEDGEMENTS
Project financed under the program the Minister of Education
and Science called “Regional Initiative of Excellence” in the
years 2019–2023, project no. 024/RID/2018/19, amount of
financing 11 999 000,00 PLN
REFERENCES (38)
1.
Biousse V, Nahab F, Newman NJ. Management of Acute Retinal Ischemia: Follow the Guidelines! Ophthalmology. 2018;125(10):1597–1607. doi:10.1016/j.ophtha.2018.03.054.
2.
Mac Grory B, Schrag M, Biousse V, et al. Management of Central Retinal Artery Occlusion: A Scientific Statement From the American Heart Association Stroke. 2021;52(6):e282–e294. doi:10.1161/STR.0000000000000366.
3.
Callizo J, Feltgen N, Pantenburg S, et al. Cardiovascular Risk Factors in Central Retinal Artery Occlusion: Results of a Prospective and Standardized Medical Examination. Ophthalmology. 2015;122(9):1881–1888. doi:10.1016/j.ophtha.2015.05.044.
4.
Feltgen N, Liman J, Schultheiss M, et al. Retinaler nichtarteriitischer Zentralarterienverschluss als Marker für das generalisierte vaskuläre Risiko [Nonaretritic central retinal artery occlusion as marker for the generalized vascular risk]. Ophthalmologe. 2021;118(11):1093–1098. doi:10.1007/s00347-021-01466-6.
5.
Hayreh SS, Podhajsky PA, Zimmerman MB. Retinal artery occlusion: associated systemic and ophthalmic abnormalities. Ophthalmology. 2009;116(10):1928–1936. doi:10.1016/j.ophtha.2009.03.006.
6.
Rim TH, Han J, Choi YS, et al. Retinal Artery Occlusion and the Risk of Stroke Development: Twelve-Year Nationwide Cohort Study. Stroke. 2016;47(2):376–382. doi:10.1161/STROKEAHA.115.010828.
7.
Vonderlin N, Kortuem K, Siebermair J, et al. Central retinal artery occlusion as a first sign of atrial fibrillation: A 3-year retrospective single-centre analysis. Clin Cardiol. 2021;44(12):1654–1661. doi:10.1002/clc.23673.
8.
Lorentzen SE. Occlusion of the central retinal artery. A follow-up. Acta Ophthalmol (Copenh). 1969;47(3):690–703. doi:10.1111/j.1755-3768.1969.tb08157.x.
9.
Chang YS, Jan RL, Weng SF, et al. Retinal artery occlusion and the 3-year risk of stroke in Taiwan: a nationwide population-based study. Am J Ophthalmol. 2012;154(4):645–652.e1. doi:10.1016/j.ajo.2012.03.046.
10.
Chang YS, Chu CC, Weng SF, et al. The risk of acute coronary syndrome after retinal artery occlusion: a population-based cohort study. Br J Ophthalmol. 2015;99(2):227–231. doi:10.1136/bjophthalmol-2014-305451.
11.
French DD, Margo CE, Greenberg PB. Ischemic Stroke Risk in Medicare Beneficiaries with Central Retinal Artery Occlusion: A Retrospective Cohort Study. Ophthalmol Ther. 2018;7(1):125–131. doi:10.1007/s40123-018-0126-x.
12.
Vestergaard N, Torp-Pedersen C, Vorum H, et al. Risk of Stroke, Myocardial Infarction, and Death Among Patients With Retinal Artery Occlusion and the Effect of Antithrombotic Treatment. Transl Vis Sci Technol. 2021;10(11):2. doi:10.1167/tvst.10.11.2.
13.
Meer E, Scoles D, Hua P, et al. Recent Practice Patterns in Acute Retinal Artery Occlusions in the United States. Ophthalmic Epidemiol. 2022;29(6):696–702. doi:10.1080/09286586.2021.2020297.
14.
Hoyer C, Kahlert C, Güney R, et al. Central retinal artery occlusion as a neuro-ophthalmological emergency: the need to raise public awareness. Eur J Neurol. 2021;28(6):2111–2114. doi:10.1111/ene.14735.
15.
Hankey GJ, Slattery JM, Warlow CP. Prognosis and prognostic factors of retinal infarction: a prospective cohort study. BMJ. 1991;302(6775):499–504. doi:10.1136/bmj.302.6775.499.
16.
Savino PJ, Glaser JS, Cassady J. Retinal stroke. Is the patient at risk? Arch Ophthalmol. 1977;95(7):1185–1189. doi:10.1001/archopht.1977.04450070083005.
17.
Pfaffenbach DD, Hollenhorst RW. Morbidity and survivorship of patients with embolic cholesterol crystals in the ocular fundus. Am J Ophthalmol. 1973;75(1):66–72. doi:10.1016/0002-9394(73)90653-3.
18.
Dunlap AB, Kosmorsky GS, Kashyap VS. The fate of patients with retinal artery occlusion and Hollenhorst plaque. J Vasc Surg. 2007;46(6):1125–1129. doi:10.1016/j.jvs.2007.07.054.
19.
Bruno A, Jones WL, Austin JK, et al. Vascular outcome in men with asymptomatic retinal cholesterol emboli. A cohort study. Ann Intern Med. 1995;122(4):249–253. doi:10.7326/0003-4819-122-4-199502150-00002.
20.
De Potter P, Zografos L. Survival prognosis of patients with retinal artery occlusion and associated carotid artery disease. Graefes Arch Clin Exp Ophthalmol. 1993;231(4):212–216. doi:10.1007/BF00918843.
21.
Hong JH, Sohn SI, Kwak J, et al. Retinal artery occlusion and associated recurrent vascular risk with underlying etiologies. PLoS One. 2017;12(6):e0177663. doi:10.1371/journal.pone.0177663.
22.
Laczynski DJ, Gallop J, Lyden SP, et al. Retinal artery occlusion does not portend an increased risk of stroke. J Vasc Surg. 2020;72(1):198–203. doi:10.1016/j.jvs.2019.08.279.
23.
Lavin P, Patrylo M, Hollar M, et al. Stroke Risk and Risk Factors in Patients With Central Retinal Artery Occlusion. Am J Ophthalmol. 2018;196:96–100. doi:10.1016/j.ajo.2018.08.027.
24.
Mir TA, Arham AZ, Fang W, et al. Acute Vascular Ischemic Events in Patients With Central Retinal Artery Occlusion in the United States: A Nationwide Study 2003–2014. Am J Ophthalmol. 2019;200:179–186. doi:10.1016/j.ajo.2019.01.009.
25.
Wang JJ, Cugati S, Knudtson MD, et al. Retinal arteriolar emboli and long-term mortality: pooled data analysis from two older populations. Stroke. 2006;37(7):1833–1836. doi:10.1161/01.STR.0000226929.23297.75.
26.
Schorr EM, Rossi KC, Stein LK, et al. Characteristics and Outcomes of Retinal Artery Occlusion: Nationally Representative Data. Stroke. 2020;51(3):800–807. doi:10.1161/STROKEAHA.119.027034.
27.
Suri K, Majmundar M, Kumar A, et al. Outcomes and Readmission in Patients With Retinal Artery Occlusion (from the Nationwide Readmission Database). Am J Cardiol. 2022;183:105–108. doi:10.1016/j.amjcard.2022.07.040.
28.
Roskal-Wałek J, Wałek P, Biskup M, et al. Retinal Artery Occlusion and Its Impact on the Incidence of Stroke, Myocardial Infarction, and All-Cause Mortality during 12-Year Follow-Up. J Clin Med. 2022;11(14):4076. Published 2022 Jul 14. doi:10.3390/jcm11144076.
29.
Hwang DDJ, Lee KE, Kim Y, et al. Incidence of Retinal Artery Occlusion and Related Mortality in Korea, 2005 to 2018. JAMA Network Open, 2023;6(3):e233068-e233068.
30.
Woo SC, Lip GY, Lip PL. Associations of retinal artery occlusion and retinal vein occlusion to mortality, stroke, and myocardial infarction: a systematic review. Eye (Lond). 2016 Aug;30(8):1031–8. doi: 10.1038/eye.2016.111. Epub 2016 Jun 3. PMID: 27256303; PMCID: PMC4985669.
31.
Gattringer T, Posekany A, Niederkorn K, et al. Predicting Early Mortality of Acute Ischemic Stroke. Stroke. 2019;50(2):349–356. doi:10.1161/STROKEAHA.118.022863.
32.
Prencipe M, Culasso F, Rasura M, et al. Long-term prognosis after a minor stroke: 10-year mortality and major stroke recurrence rates in a hospital-based cohort. Stroke. 1998;29(1):126–132. doi:10.1161/01.str.29.1.126.
33.
Roskal-Wałek J, Mackiewicz J, Wałek P, et al. Retinal artery occlusion and its association with stroke –literature review. Medical Studies/Studia Medyczne. 2023;39(1):55–64. doi:10.5114/ms.2023.126296.
34.
Fallico M, Lotery AJ, Longo A, et al. Risk of acute stroke in patients with retinal artery occlusion: a systematic review and meta-analysis. Eye (Lond). 2020;34(4):683–689. doi:10.1038/s41433-019-0576-y.
35.
Bokura H, Kobayashi S, Yamaguchi S, et al. Silent brain infarction and subcortical white matter lesions increase the risk of stroke and mortality: a prospective cohort study. J Stroke Cerebrovasc Dis. 2006;15(2):57–63. doi:10.1016/j.jstrokecerebrovasdis.2005.11.001.
36.
Windham BG, Deere B, Griswold ME, et al. Small Brain Lesions and Incident Stroke and Mortality: A Cohort Study. Ann Intern Med. 2015;163(1):22–31. doi:10.7326/M14-2057.
37.
Kang EY, Lin YH, Wang NK, et al. Aspirin use in central retinal arterial occlusion to prevent ischaemic stroke: a retrospective cohort study in Taiwan. BMJ Open. 2019;9(2):e025455. doi:10.1136/bmjopen-2018-025455.
38.
Roskal-Wałek J, Wałek P, Biskup M, et al. Central and Branch Retinal Artery Occlusion-Do They Harbor the Same Risk of Further Ischemic Events? J Clin Med. 2021;10(14):3093. doi:10.3390/jcm10143093.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.