Online first
Current issue
Archive
Special Issues
About the Journal
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Board
Editorial Office
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
RESEARCH PAPER
Epidemiology of carbapenem-resistant Klebsiella pneumoniae in healthcare-associated
infections – a retrospective study from Taiwan
1
Department of Computer Science and Information Engineering, National Chin-Yi University of Technology, Taichung, Taiwan
2
Department of Post-Baccalaureate Programme in Nursing, Central Taiwan University of Science and Technology, Taichung, Taiwan
Corresponding author
Kuan-Yu Lin
Department of Post-Baccalaureate Programme in Nursing, Central University of Science and Technology, Taiwan
Department of Post-Baccalaureate Programme in Nursing, Central University of Science and Technology, Taiwan
Ann Agric Environ Med. 2025;32(3):335-339
KEYWORDS
TOPICS
- Biological agents posing occupational risk in agriculture, forestry, food industry and wood industry and diseases caused by these agents (zoonoses, allergic and immunotoxic diseases)
- State of the health of rural communities depending on various factors: social factors, accessibility of medical care, etc.
ABSTRACT
Introduction and objective:
In recent years, carbapenem-resistant Enterobacteriaceae, particularly carbapenem-resistant Klebsiella pneumoniae (CRKP), have emerged as a global public health concern, posing substantial challenges to clinical treatment. The aimof the study is to investigate the prevalence of CRKP in healthcare-associated infections (HAIs), and to support the development of effective surveillance mechanisms and antimicrobial resistance containment strategies.
Material and methods:
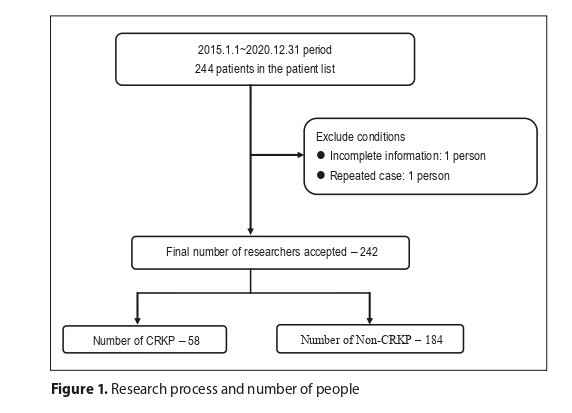
A retrospective observational study was conducted using HAI data from a medical centre in central Taiwan, covering the period from January 2015 to December 2020. Cases of Klebsiella pneumoniae infection were categorized into two groups: CRKP (case group) and non-CRKP (control group). Risk factors were assessed using Pearson’s χ2 test or continuity correction (Fisher’s exact); a t‑test was applied alongside univariable and multivariable logistic regression analyses.
Results:
Results indicated a high prevalence of CRKP in patients with cardiovascular disease (odds ratio [OR] = 3.33; 95% confidence interval [CI]: 1.24–8.97; p =.017), prior exposure to carbapenems (OR = 3.70; 95% CI: 1.69–8.10; p =.001), presence of urinary catheters (OR = 3.51; 95% CI: 1.30–9.50; p =.013), and haemodialysis catheters (OR = 6.57; 95% CI: 2.17–19.91; p =.001).
Conclusions:
The incidence of CRKP-related HAIs demonstrated an upward trend over the study period. These findings suggest that patients with cardiovascular disease, or those requiring urinary or haemodialysis catheters, should avoid unnecessary invasive procedures. Enhanced monitoring and control of CRKP strains are imperative for preventing the emergence and spread of multi-drug-resistant and hypervirulent variants.
In recent years, carbapenem-resistant Enterobacteriaceae, particularly carbapenem-resistant Klebsiella pneumoniae (CRKP), have emerged as a global public health concern, posing substantial challenges to clinical treatment. The aimof the study is to investigate the prevalence of CRKP in healthcare-associated infections (HAIs), and to support the development of effective surveillance mechanisms and antimicrobial resistance containment strategies.
Material and methods:
A retrospective observational study was conducted using HAI data from a medical centre in central Taiwan, covering the period from January 2015 to December 2020. Cases of Klebsiella pneumoniae infection were categorized into two groups: CRKP (case group) and non-CRKP (control group). Risk factors were assessed using Pearson’s χ2 test or continuity correction (Fisher’s exact); a t‑test was applied alongside univariable and multivariable logistic regression analyses.
Results:
Results indicated a high prevalence of CRKP in patients with cardiovascular disease (odds ratio [OR] = 3.33; 95% confidence interval [CI]: 1.24–8.97; p =.017), prior exposure to carbapenems (OR = 3.70; 95% CI: 1.69–8.10; p =.001), presence of urinary catheters (OR = 3.51; 95% CI: 1.30–9.50; p =.013), and haemodialysis catheters (OR = 6.57; 95% CI: 2.17–19.91; p =.001).
Conclusions:
The incidence of CRKP-related HAIs demonstrated an upward trend over the study period. These findings suggest that patients with cardiovascular disease, or those requiring urinary or haemodialysis catheters, should avoid unnecessary invasive procedures. Enhanced monitoring and control of CRKP strains are imperative for preventing the emergence and spread of multi-drug-resistant and hypervirulent variants.
REFERENCES (17)
1.
Zhu L, Liang L, Hui J, et al. Relationship between antibiotic exposure and carbapenem-resistant Klebsiella pneumoniae infection within four types of control patients: A systematic review and meta-analysis. J Glob Antimicrob Resist. 2023;33:137–151.
2.
Pu D, Zhao J, Chang K, et al. “Superbugs” with hypervirulence and carbapenem resistance in Klebsiella pneumoniae: the rise of such emerging nosocomial pathogens in China. Sci Bull (Beijing). 2023;68:2658–2670.
3.
Han YL, Wen XH, Zhao W, et al. Epidemiological characteristics and molecular evolution mechanisms of carbapenem-resistant hypervirulent Klebsiella pneumoniae. Front Microbiol. 2022;13:1003783.
4.
Qin X, Wu S, Hao M, et al. The Colonization of Carbapenem-Resistant Klebsiella pneumoniae: Epidemiology, Resistance Mechanisms, and Risk Factors in Patients Admitted to Intensive Care Units in China. J Infect Dis. 2020;221:S206–S214.
5.
Hsu JY, Chuang YC, Wang JT, et al. Healthcare-associated carbapenem-resistant Klebsiella pneumoniae bloodstream infections: Risk factors, mortality, and antimicrobial susceptibility, 2017–2019. J Formos Med Assoc. 2021;120:1994–2002.
6.
Mazzeffi M, Galvagno S, Rock C. Prevention of Healthcare-associated Infections in Intensive Care Unit Patients. Anesthesiology. 2021;135:1122–1131.
7.
Yao Y, Zha Z, Li L, et al. Healthcare-associated carbapenem-resistant Klebsiella pneumoniae infections are associated with higher mortality compared to carbapenem-susceptible K. pneumoniae infections in the intensive care unit: a retrospective cohort study. J Hosp Infect. 2024;148:30–38.
8.
Lakoh S, Li L, Sevalie S, et al. Antibiotic resistance in patients with clinical features of healthcare-associated infections in an urban tertiary hospital in Sierra Leone: a cross-sectional study. Antimicrob Resist Infect Control. 2020;9:38.
9.
Blot S, Ruppé E, Harbarth S, et al. Healthcare-associated infections in adult intensive care unit patients: Changes in epidemiology, diagnosis, prevention and contributions of new technologies. Intensive Crit Care Nurs. 2022;70:103227.
10.
Vanegas JM, Salazar-Ospina L, Roncancio GA, et al. Post-antibiotic era in hemodialysis? Two case reports of simultaneous colonization and bacteremia by multidrug-resistant bacteria. J Bras Nefrol. 2021;43:597–602.
11.
Li J, Li Y, Song N, Chen Y. Risk factors for carbapenem-resistant Klebsiella pneumoniae infection: A meta-analysis. J Glob Antimicrob Resist. 2020;21:306–313.
12.
Zhu WM, Yuan Z, Zhou HY. Risk factors for carbapenem-resistant Klebsiella pneumoniae infection relative to two types of control patients: a systematic review and meta-analysis. Antimicrob Resist Infect Control. 2020;9:23.
13.
Liu P, Li X, Luo M, et al. Risk Factors for Carbapenem-Resistant Klebsiella pneumoniae Infection: A Meta-Analysis. Microb Drug Resist. 2018;24:190–198.
14.
Chen Y, Chen Y, Liu P, et al. Risk factors and mortality for elderly patients with bloodstream infection of carbapenem resistance Klebsiella pneumoniae: a 10-year longitudinal study. BMC Geriatr. 2022;22:573.
15.
Wei T, Zou C, Qin J, et al. Emergence of Hypervirulent ST11-K64 Klebsiella pneumoniae Poses a Serious Clinical Threat in Older Patients. Front Public Health. 2022;10:765624.
16.
Lei J, Zhou WX, Lei K, et al. Analysis of molecular and clinical characteristics of carbapenem-resistant hypervirulent Klebsiella pneumoniae in the intensive care unit. 2022;56:63–68.
17.
Xu L, Sun X, Ma X. Systematic review and meta-analysis of mortality of patients infected with carbapenem-resistant Klebsiella pneumoniae. Ann Clin Microbiol Antimicrob. 2017;16:18.
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.