Online first
Current issue
Archive
Special Issues
About the Journal
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Board
Editorial Office
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
CASE REPORT
Cryptosporidium spp. and Blastocystis spp. coinfection as a reason of an acute diarrhea in a young healthy veterinary Polish student – Case report
1
Department of Tropical and Parasitic Diseases Medical University, Poznań, Poland
2
Central Microbiology Laboratory, H. Święcicki University Hospital, Poznań, Poland
3
Parasitology Laboratory, H.Święcicki University Hospital, Poznań, Poland
4
Central Microbiology Laboratory, J. Struś City Hospital, Poznań, Poland
Corresponding author
Łukasz Augustyn Pielok
Tropical and Parasitic Diseases Departament, Medical University, Poznań, Poland
Tropical and Parasitic Diseases Departament, Medical University, Poznań, Poland
Ann Agric Environ Med. 2022;29(4):592-594
KEYWORDS
TOPICS
- Biological agents posing occupational risk in agriculture, forestry, food industry and wood industry and diseases caused by these agents (zoonoses, allergic and immunotoxic diseases)
- Work-related accidents and injuries in agriculture, forestry, food industry and wood industry: incidence, causes, social aspects and prevention
ABSTRACT
Objectives:
Cryptosporidium belongs to enteric parasites responsible for prolonged symptoms in the gastrointestinal tract, both in immunocompetent and immunocompromised individuals. One of the risk factors of infection is contact with an infected person or animals (cattle). The case is described of a young man admitted to the Department of Tropical and Parasitic Diseases of the Medical University in Poznań, Poland, because of watery diarrhea with high fever and in whom symptomatic treatment did not produce any improvement.
Material and Methods:
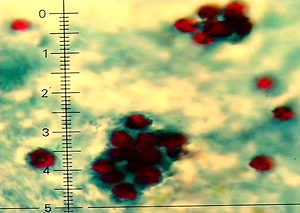
A 21-year -old male was examined and his epidemiologic history obtained. Primary blood test, anti- Toxocara IgG (ELISA) and anti-Toxoplasma gondii IgG and IgM (ELISA) were performed. PCR detected 16 enteropathogens in a stool sample. Microscopic parasitic stool examination was also performed based on Ziehl-Neelsen method, which allowed the assessment of the presence of cryptosporidium life stages.
Results:
Epidemiology data provided information that the patient was a veterinary student who therefore had many contacts with domestic animals. Multiplex PCR detected a genetic material of Cryptosporidium. The result was confirmed with repeated positive direct stool examinations which gave the evidence of Cryptosporidium spp. oocysts and vacuolar forms of Blastocystis spp.
Conclusions:
1) Cryptosporidium is responsible for watery diarrhea in healthy individuals. 2) Contact with animals (cattle) is a potential risk factor for infection. 3) Protozoan co-infection should be treated to shorten the symptomatic period and to avoid post-infection complications. 4) Different diagnostic methods increase the possibility to establish appropriate diagnosis
Cryptosporidium belongs to enteric parasites responsible for prolonged symptoms in the gastrointestinal tract, both in immunocompetent and immunocompromised individuals. One of the risk factors of infection is contact with an infected person or animals (cattle). The case is described of a young man admitted to the Department of Tropical and Parasitic Diseases of the Medical University in Poznań, Poland, because of watery diarrhea with high fever and in whom symptomatic treatment did not produce any improvement.
Material and Methods:
A 21-year -old male was examined and his epidemiologic history obtained. Primary blood test, anti- Toxocara IgG (ELISA) and anti-Toxoplasma gondii IgG and IgM (ELISA) were performed. PCR detected 16 enteropathogens in a stool sample. Microscopic parasitic stool examination was also performed based on Ziehl-Neelsen method, which allowed the assessment of the presence of cryptosporidium life stages.
Results:
Epidemiology data provided information that the patient was a veterinary student who therefore had many contacts with domestic animals. Multiplex PCR detected a genetic material of Cryptosporidium. The result was confirmed with repeated positive direct stool examinations which gave the evidence of Cryptosporidium spp. oocysts and vacuolar forms of Blastocystis spp.
Conclusions:
1) Cryptosporidium is responsible for watery diarrhea in healthy individuals. 2) Contact with animals (cattle) is a potential risk factor for infection. 3) Protozoan co-infection should be treated to shorten the symptomatic period and to avoid post-infection complications. 4) Different diagnostic methods increase the possibility to establish appropriate diagnosis
REFERENCES (20)
1.
Rzeżutka A, Kaupke A, Gorzkowski B. Detection of Cryptosporidium parvum in a Red-Eared Slider-Turtle (Trachemys scripta elegans), a Noted Invasive Alien Species, catured in a Rural Aquatic Ecosystem in Eastern Poland. Acta Parasitol.2020 Sep;65(3):768–773. doi:102478/s11686-020-00180-8.Epub2020 Mar5.
2.
Cassio SM, Pozio E. Advences in the epidemiology, diagnosis and treatment of cryptosporidiosis. Expert Rev Anti Infect Ther. 2006 Jun;4(3):429–43. doi:10.1586/14787210.4.3.4293.
3.
Pielok Ł, Nowak SzP, Kłudkowska M, Frąckowiak K, Kuszel Ł, Zmora P, Stefaniak J. Massive Cryptosporidium infection and chronic diarrhea in HIV-negative patients. Parasitol Res. 2019 Jun;118(6):1937–1942. doi:10.1007/s00436-019-0632-0.
4.
Bouzid M, Hunter PR, Chalmers RM, Tyler KM. Cryptosporidium pathogenicity and virulence. Clin Microbiol Rev. 2013 Jan;26(1):115–34. doi:10.1128/CMR.00076-12.
5.
Tallant C, Huddleston P, Alshanbesi A, Misra S. Acuye, Cever Cryptosporidiosis in an Immunocometent Pediatric Patient. Clin Pract. 2016 Jul 4;6(2):837. doi:10.4081/cp.2016.837.eCollection 2016 Apr.26.
6.
Ryan U, Zahedi A, Papanini A. Cryptosporidiosis in humans and animals – a one health approach to prophylaxis. Parasite Immunol. 2016 Sep;38(9):535–47. doi:10.1111/pim.12350.
7.
Tzipori S, Ward H. Cryptosporidiosis: biology, pathogenesis and disease. Microbes Infect. 2002 Aug;4(10):1047–58. doi:10.1016/s1286-4579(2)01629-5.
8.
Hossa EM, Omeci B, DeRosa MC, Dixon BR, Sattar SA, Igbal A. A review of Cryptosporidium spp. and their detection in water. Water Sci Technol.2021 Jan;83(1):1–25. doi:10.2166/wst.2020.515.
9.
Fayer R. Cryptosporidium: a water-borne zoonotic parasite. Vet Parasitol. 2004 Dec 9;126 (1–2):37–56. doi:10.1010/i.vetpar.2004.09.004.
10.
Chalmers RM, Alexander C. Defining the diagnosis of cryptosporidiosis. Lancet Infect Dis. 2021 May;21(5):589–590. doi:10.1016/S1473-3099(20)30575-2.
11.
Kothavade RJ. Challenges in understanding the immunopathogenesis of Cryptosporidiosis in human. J Clin Microbiol Infect Dis. 2011 Dec;30(12):1461–72.
12.
Gaul R, Soutar RH, Hanson M, Fraser C, Chalmers R. Outbreak of Cryptosporidiois among veterinary students. Vet Rec. 2008 Jun 28;162(26):843–5. doi:10.1136/vr.162.26.843.
13.
Kiuross P, Beser J, Troell K, Axen C, Bjornkman C, Lebbad M, Winiecka-Kruszel j, Lindth J, Lofdahl M. Cryptosporidium parvum infections in a cohort of veterinary students in Sweden. Epidemiol Infect. 2015 Oct;143(13):2748–56. doi:10.1017/S0950268814003318.
14.
Caccis SM, Chalmers RM. Human cryptosporidiosis in Europe. Clin Microbiol Infect. 2016 Jun;22(6):471–80. doi:10.1016/j.cmi.2016.04.021.
15.
Chako CZ, Tyler JW, Schultz LG, Chiguma L, Beernitsen BT. Cryptosporidiosis in People: It’s Not Just About the Cows. J Vet Intern Med. Jan-Feb 2010;24(1):37–43. doi:10.1111/j.1939-1676.2009.0431.x.
16.
Pantenburg B, Cabade M, White Jr AC. Treatment of cryptosporidiosis. Exper Rev Anti Infect Ther. 2009 May; 7(4):385–91. doi:10.1586/eri.24.
17.
Tahvildar-Biderouni F, Salehi N. detection of Cryptosporidium infection by modified Ziehl-Neelsen and PCR methods in children with diarrheal samples in pediatric hospitals in Teheran. Gastroenterol Hepatol Bed Bench. 2014 Spring:7(2):125–130.
18.
Duda A, Kosik-Bogacka D, Lanocka N, Szymański S. Blastocystis hominis parasites or commensals. Ann Acad MedStetin. 2014;60(1):23–8.
19.
Taghipour A, Rayatdoost E, Bairami A, Bahadory S, Abdali A. Are Blastocystis hominis and Cryptosporidium spp. playing a positive role in colorectal cancer risk? A systemic review and meta analysis. Infect Agent cancer. 2020 Jun 17;17(1):32. doi:10.1186/s13027-022-00447-x.
20.
Yellanthoor RB. Acute gastroenteritis due to Blastocystis hominis in an adolescent boy. BMJ Case Rep.2020.Dec21;13(12):e237810. doi:101136/bcr-2020-237810.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.